|
Changing mindset is one of the most powerful ways to mitigate stress. Carol Dweck, a Stanford psychologist, has shown how we think about a situation will ultimately change the outcome. People with what she calls a “growth mindset” attribute mistakes and mishaps as opportunities for growth and improvement. In contrast, people with “fixed mindsets” are more apt to give up and attribute their shortcomings to character traits or fixed variables that they have little influence over changing or improving.  Photo by sydney Rae on Unsplash At Wellness Garage, we encourage our members to adopt a “The Better Mindset”:
'small changes, done consistently, lead to massive results over time.' In other words, people can improve by doing better in small ways:
When the situation challenges you, and you cannot fit in a workout, eat well, or get your 8 hours of sleep, the better mindset helps you find something you can do better than what could have been. When things don’t go well, the “better mindset” allows you to reflect and learn from the situation to plan better next time. When you fall off track, the “better mindset” reminds you that tomorrow is another day to be better. Above all, the “better mindset” is about taking small steps to improve and feel good about yourself. Combining the “growth” and “better” mindsets will help you manage the multiple stressors many of us have in our lives: work, kids, family commitments, financial stressors, our health. When you find it overwhelming just managing everything in your day-to-day routines, try to shift your thinking about stress. Use the “growth” mindset to look for how you can extend control over your current situation. Instead of focusing on being overwhelmed, examine how you can learn and grow. Then take the “better” mindset and realize that you do not need to do everything perfectly; that better is better. Maybe you don’t have time to cook dinner, do your workout, help your kids with their homework, but you can order a healthy meal delivery from a local restaurant that you have meant to try, get out for a walk (instead of cooking) and help the kids. By shifting to “better” rather than “perfect,” you get the opportunity to learn new ways to manage. Whenever you find your mind sending messages of being overwhelmed or feeling powerless, try countering the thought by feeling grateful for opportunities in your life. Feel gratitude for all the good things in your life, even if together they can be a bit stressful at times. Research shows that having a “gratitude” mindset and doing the simple exercise of reciting three things you are grateful for each day will make you a happier person with less stress. We cannot control everything in life, but we do have more control over our mindset and how we interpret our stressors. By understanding your physiology, you can improve your ability to tolerate stress and thrive despite challenges. Stress is your body’s response to a perceived threat or challenge from your environment. This response is either amplified or abbreviated depending on four factors:
The last post detailed strategies to architect your lives to reduce avoidable stress and give yourself adequate time to recover from your pre-existing stress load. This post will review some techniques that can help you change your perception and mindset - to alter your perception of the stressor and immediately mitigate the response. Meditation and mindfulness Mindfulness exercises your innate ability to be fully present in the moment, simply observing thoughts, feelings and sensations as you become aware of them. This awareness is non-judgmental - you explicitly try not to interpret what you are sensing. One common mindfulness exercise is to sit quietly, with your eyes closed, breathing slowly through your nose, observing your breath as you inhale and exhale slowly. While it sounds easy, it is challenging not to judge or interpret or follow all the other thoughts and sensations that come into your mind. The key to the exercise is to simply recognize when your mind has wandered and return the focus to the breath. A common misconception of mindfulness meditation is that the goal is to stop your thoughts - this is impossible. A helpful analogy is to think of yourself sitting on the platform at a train station. The trains that enter and leave the station are your thoughts, feelings and sensations. The goal is to simply sit there and watch the trains come and go. You cannot stop the trains; they will keep coming; your job is to watch them go without getting on any of them. Of course, what happens in practice is that you get on the train, and off you go down several stops. For example, you are sitting quietly, observing your breath when you notice a sensation in your stomach. Now you get on the train. “I’m hungry...where do I want to have lunch… there is that cool cafe down the street where I went with Paul...Paul seems distracted these days...I wonder if he is upset with me...I have been really stressed and short with people the past month…” Your train of thought takes you far away from your focus on your breath. Here is the key - your job is simply to get off the train and return to the platform - resuming your focus on breathing in and breathing out. It is this ability to return to the awareness of the moment that can become your super-power. Like so many healthy lifestyle behaviours, mindfulness meditation is pretty simple but very difficult. It takes practice. Fully developed, your ability to stay in the moment will reduce stress by changing your perception of threats. Most often, it is not the particular event that is stressful; it is our interpretation: the runaway train of thoughts that causes most of the stress. Getting started with mindfulness meditation is easy - start with this exercise that combines mindfulness with a light set of yoga stretches: Nighttime Yoga & Mindfulness Practice. Another practice you can develop to change your perception of stress builds on the nature of your interpretations. Byron Katie, has come up with a simple exercise she calls “The Four Questions”.
The next time you have a stressful event - ask yourself these questions:
Then “turn it around” what other interpretations are there of what just happened - how do they make you feel. For example, let’s say you have a friend named Paul and you think he has lied to you. Are you sure? Could Paul just be mistaken, are you sure that he has lied? How do you feel? “Betrayed, hurt - why do my friends always lie to me... they are jealous of me, they don’t respect me…” “I would feel so much better if I didn’t feel this way. I am a good friend.” Now turn it around, tell yourself another story about the same situation: “Paul was telling a white lie to save my feelings..he is a good friend who was looking out for me...I am fortunate to have friends that are sensitive to my feelings.” The simplicity and accessibility of the “Four Questions” technique makes it very powerful. Doing this once or twice, helps you to realize in the moment when you are jumping on the train. Most of our stress comes from the story we tell ourselves about the event - not the actual event. Like mindfulness, the “Four Questions” becomes a useful tool in your stress tolerance toolkit to avoid magnifying stress with runaway thoughts. In our next post, we will turn to the role of mindset to help with stress tolerance. With an understanding that you probably aren’t able to alter many of your underlying allostatic load factors :
What changes can you make to establish the foundation for a calmer, lighter future? How can you Architect Your Life, reducing or avoiding predictable stressors, and building more space for recovery? To accept the things I cannot change; courage to change the things I can; and wisdom to know the difference." - Serenity Prayer Here are two techniques that can be very helpful, the first a foundational pro-active approach and the second an ongoing regular process.
The first technique will take some time (but it is a game-changer if you do it) this is the Time-Values Audit:
Try this four-step strategy to architect a life that allows for stress recovery:
Our second technique is simpler: Regularly review your weekly calendar how you spend your time.
Now with this reflection fresh in your mind, plan your next week - what can you do (or not do) to make it flow better, align with your values and avoid predictable stress. This is the second post in our STRESSRecovery guide. Click here to read the first post. That which does not kill us makes us stronger - (Friedrich Nietzsche) ...provided we get enough recovery - (Wellness Garage) When we hear the term stress, we think of the harm it does. And in fact, chronic stress plays a central role in the development and progression of chronic disease and ill health. Yet stress provides the signal to adapt to life’s challenges, increasing our fitness and allowing us to thrive. This is the double-edge of of stress, the paradox that it can both protect and damage. Balancing our stress with adequate recovery tilts the balance in favour of resilience and good health. Stress is a response to perceived threats or challenges from our environment. We perceive that the stressor will harm us, and our brains mobilize a response to protect us. When we perceive a threat, our bodies respond by:
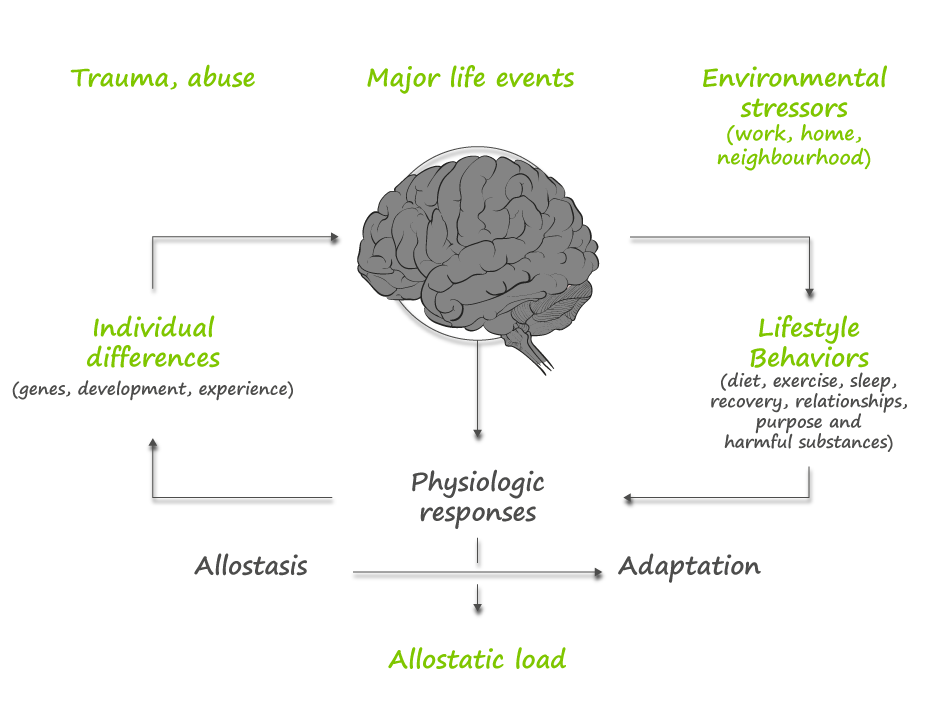
From an evolutionary perspective, these challenges tended to be life-threatening hence the term “fight, flight or freeze.” In the modern world, stressors are often more psychological than physical, are more frequent and last longer. This evolutionary mismatch between our biology and our current environment is why chronic stress has become epidemic and is responsible for many symptoms and illnesses that we see in practice today. The magnitude of our stress response always depends on our perception, which can be both instinctual and a conditioned response to previous experiences. Beyond this immediate perception of threat, many other life factors determine our response:
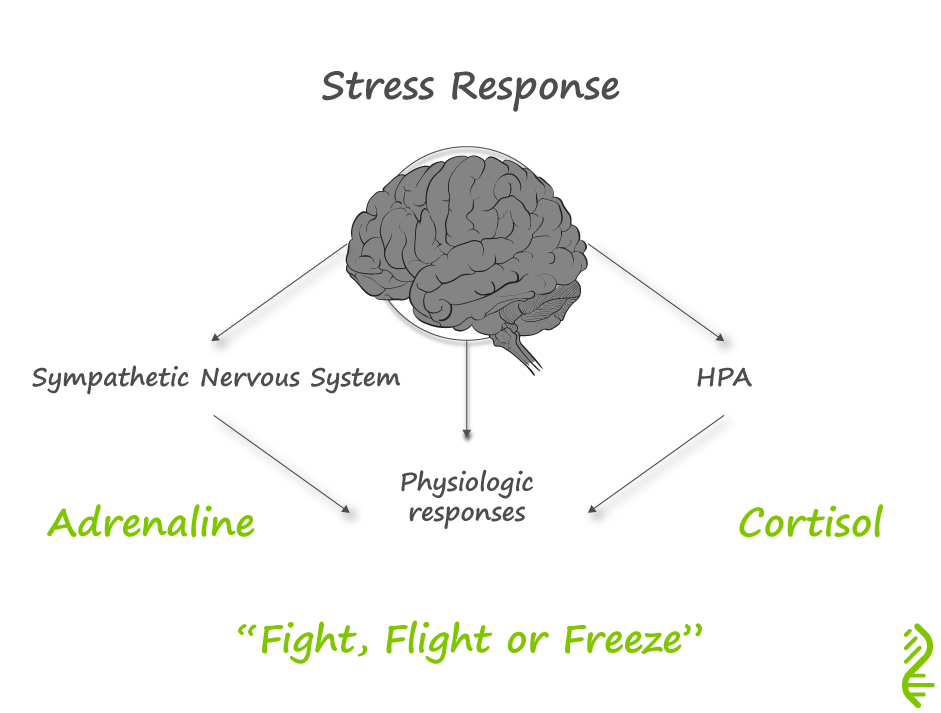
It is this net perception of stress which determines the extent of our physiological response. The amygdala, deep in the temporal lobes of our brain, integrates our perception of the stressor and triggers our physiological response by signalling our hypothalamus. In turn, the hypothalamus triggers the sympathetic nervous system, which then activates the inner part of the adrenal gland to release adrenaline resulting in:
We feel this combination of physiological effects as an ‘adrenaline rush’. The hypothalamus also releases the hormone CRH, which activates the pituitary gland to secrete adrenocorticotropic hormone (ACTH) that stimulates the adrenal gland’s outer part to produce cortisol. Cortisol enables the body to maintain steady supplies of blood sugar for more prolonged stress. Adequate and steady blood sugar levels help us cope with prolonged stressors and help the body to return to normal. Cortisol does this by:
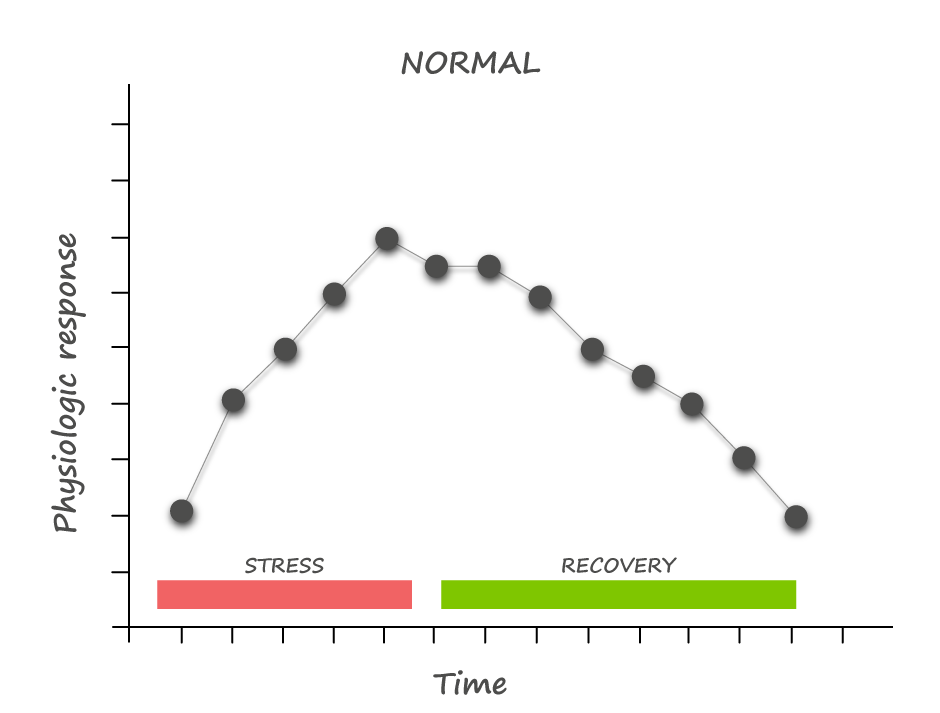
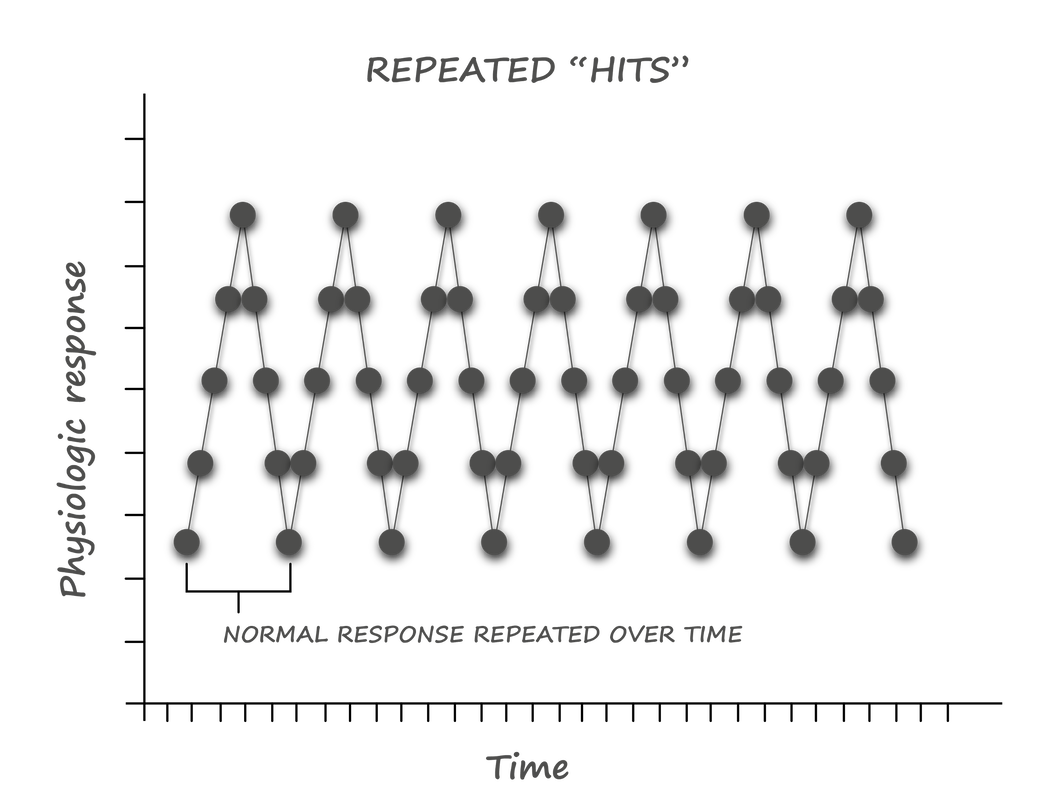
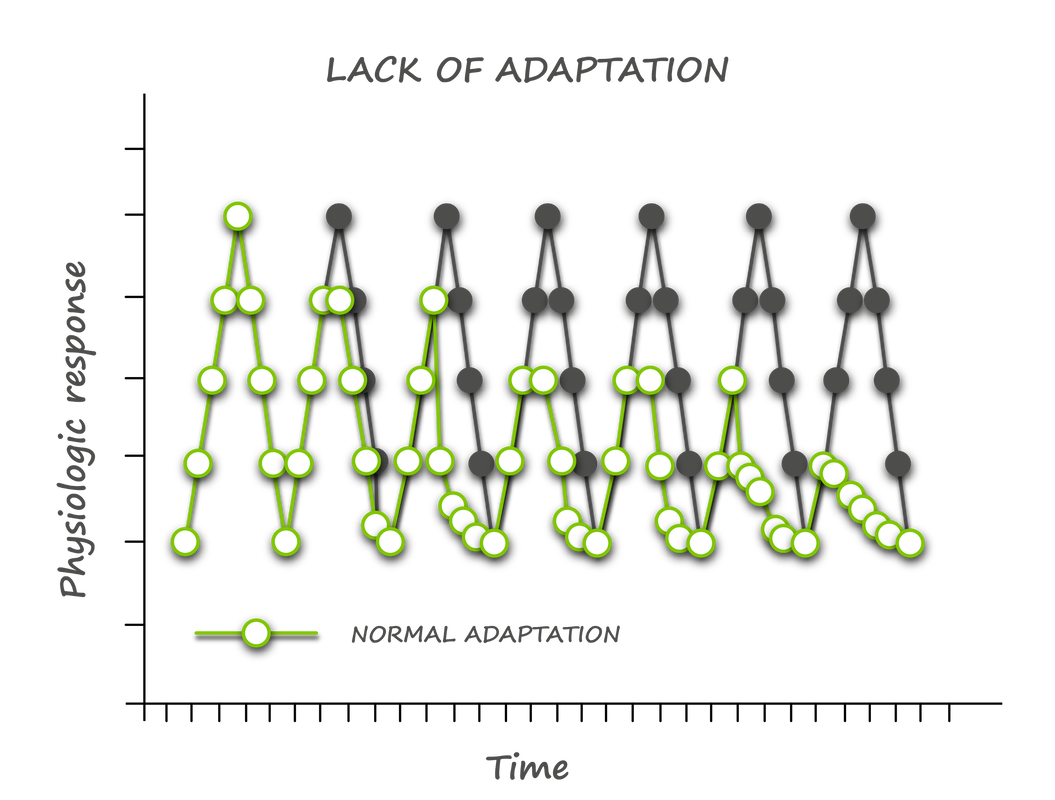
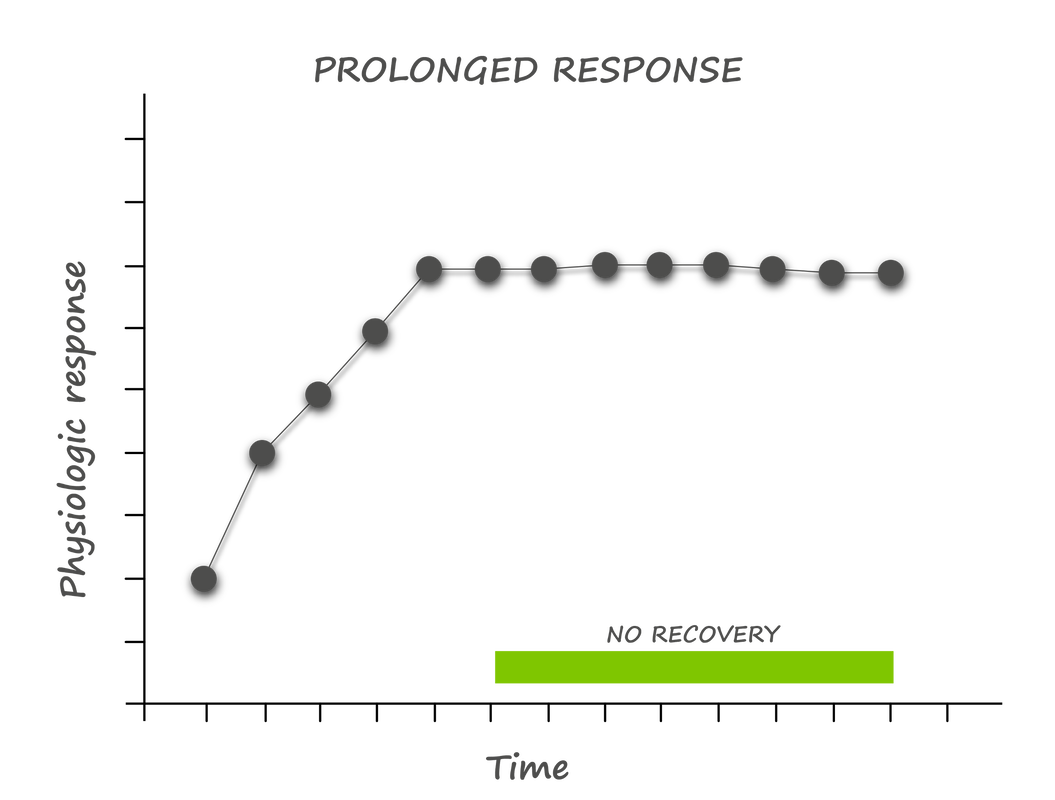
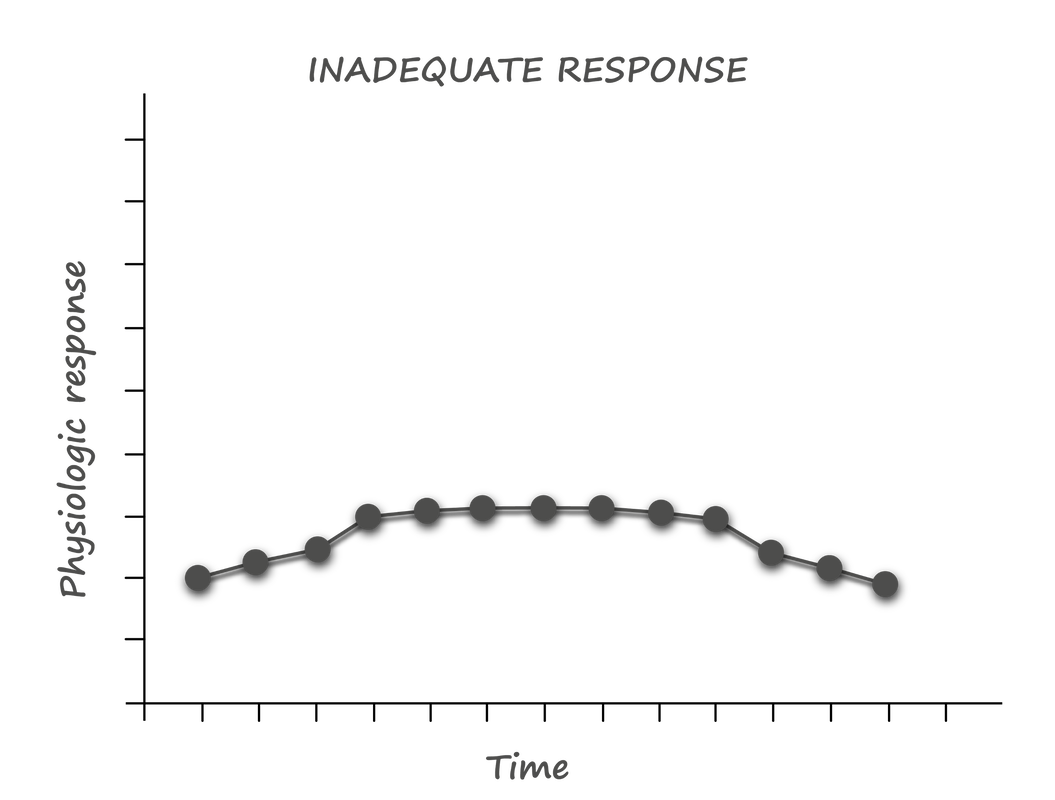
Prolonged psychological stress drives the same response; however, the mobilization of energy has little purpose. Without activity, most of this mobilized energy turns into visceral fat - the metabolically unfavourable fat associated with insulin resistance. This phenomenon explains the belly fat accumulated in stressed-out executives and explains how stress can lead to metabolic dysfunction and Type II Diabetes. Recovery When the stressor passes, our bodies initiate a recovery response, activating the parasympathetic nervous system and turning off the production of adrenaline and cortisol. With full recovery, our bodies make adjustments and adaptations that can make us stronger. This whole process is called allostasis - the ability to achieve stability through change. How things go wrong When these acute responses are overused or inefficiently managed, instead of adaptation, allostatic overload results. There are four patterns to the accumulation of allostatic overload: 1. Repeated "hits" from multiple novel stressors 2. Lack of adaptation to a single repetitive stressor 3. Prolonged stress without recovery 4. An inadequate stress response that leads to compensatory hyperactivity of other systems - especially the inflammatory pathway With this understanding of the underlying physiology, it becomes clear that four factors determine our responses to potential stressors:
Developing strategies that address these four factors can decrease the stress response and improve recovery:
The next five posts will detail these strategies and pull them all together as a healthy, lifestyle approach to improving stress tolerance. One of the most common reasons people increase activity is to burn more calories, create a calorie deficit, and lose weight. A new study demonstrates that this might not work as simply as we think. Using the most extensive dataset on human energy expenditure ever assembled ( n = 1754), researchers demonstrated that increasing activity is compensated by a decrease in basal or resting energy expenditure. So for every 100 calories of additional activity, we only burn 72 calories - a compensation of 28%. This relationship was similar for men and women, young and old. Making matters worse for people seeking to lose weight through increased energy expenditure is the observation that the level of compensation increases with weight. People at the 90th percentile weight (BMI = 33) in this study compensate almost half of their calories. Finally, there is a significant variation amongst people - some compensate more or less than others.  Photo by Shoeib Abolhassani on Unsplash This finding has several implications:
The potential relationship between the increase in appetite associated with increased activity and this energy compensation was not touched upon in the study but has significant real-world implications. The increase in appetite (and consumption) for some people may be equal or potentially greater than the increase in actual calories burned. These combined effects may be why exercise alone generally does not work for significant weight loss. Another potential implication not touched upon in the study is that the compensatory decrease in energy expenditure may have possible health benefits (i.e. decreased immune system activity, decreasing chronic inflammation). This may be one reason why exercise has been shown to have such significant health benefits despite its lack of efficacy for weight loss. As humans, we are designed to respond to stress through a process called allostasis- “maintaining stability through altering physiologic parameters to counteract challenges.”
We all have a built-in stress response, where the sympathetic nervous system (SNS) activates for short periods to address short-term stressors. When the SNS is in charge, the body prepares for fight, flight or freeze. During this time, adrenaline and cortisol flood the bloodstream, the heart rate increases, digestion slows, and breathing becomes rapid. We are ready for whatever life throws at us! When the stressor passes, the relaxation response - our parasympathetic nervous system - the one responsible for rest and relaxation - kicks in, and our bodies return to normal. This alternating pattern of sympathetic and parasympathetic nervous system activation is the natural cycle that we all experience when encountering stress. But what if the stressor doesn’t pass? Peter A. Levine, a trauma researcher, has studied animals in the wild who are constantly exposed to external threats (stressors). He found that when animals draw on heightened amounts of energy, they have mechanisms to release the excess energy through behaviours such as shaking, running or bucking. Humans, on the other hand, don’t have built-in systems for trauma and stress. Hence, chronic stress over time erodes our resilience. Levine notes that when a stressor never passes- due to either external events or our internal response to those events, the SNS gets flipped and “stays on”- not fully returning to a state of rest and relaxation. The result is called allostatic overload and directly connects to a decline in physical and mental health. Fortunately for us as humans, we have other mechanisms to counter stress - beyond that of animals. So next time you feel that your body and mind are in a heightened state, being overrun by your SNS, try these tools to reset: 1. Breathe Breathing is the only part of the parasympathetic nervous system that we can control as humans. Resonant Breathing- deep breathing in and out at a methodical pace (3-7 breaths per minute) has been shown to improve symptoms of depression and anxiety. 2. Take a Walk In Nature: Shinrin-Yoku is the ancient Japanese tradition of walking in the forest while engaging the senses. The English translation- forest bathing- has become popular in treating various lifestyle diseases and has been shown to improve immune function and promote an overall sense of calm. 3. Fill your plate with Healthy Whole Foods: Research on ‘food and mood’ has linked specific nutrients- such as Omega 3s- found in fish, walnuts and soybeans- to improved mental health. Other foods such as whole grains, colourful veggies and fermented foods support a healthy gut and microbiome. Growing research points to the role a healthy gut plays in maintaining mental health. Check out our EATBetter guide. 4. Move, Move, Move: Just 150 minutes of moderate to vigorous exercise a week is linked to a greater sense of well-being. In some studies, exercise has been shown to be as effective as medication in treating depression and anxiety. . .need we say more! Check out our LEVELUp your fitness guide. 5. Practice Mindfulness in the moment: Focus on where you are in the moment, rather than allowing the “what ifs’ of life to constantly creep into your daily thoughts. When you find your mind wandering or, in some cases spiralling- allow yourself to come back to the present moment by focusing on your five senses. Look at what you see, listen to what you hear, feel your feet on the ground, take a deep breath, smell your surroundings, and taste what is in your mouth. Check out the countless mindfulness apps to help you develop and deepen a mindfulness/ meditation practice. Finally- be sure to give yourself scheduled time to get a break from the constant stressors of life - take a bath, go for a walk, read a book, spend time with loved ones, take a holiday!! Wellness Garage will be closed from August 23rd- 29th. We look forward to seeing you again- well-rested and rejuvenated! (This post was originally shared in our RCMP Newsletter - Protect Your Health)
Post-traumatic stress disorder is a severe psychological condition that develops in response to traumatic events that often leads to chronic, disabling symptoms lasting years or decades after the trauma. PTSD is characterized by intrusive flashbacks, interrupting thoughts, nightmares, sleep disturbances. Avoidance of activities, relationships or thoughts that stimulate memories of the trauma can lead to irritability, isolation, guilt and depression. A recent study estimates that 1 in 3 RCMP members currently have PTSD - almost four times the general population’s lifetime prevalence. Effective treatments are available, including counselling, psychotherapy as well as medication. Unfortunately, many people with PTSD have residual symptoms resistant to treatment and lead to long-term disability. Current treatments all focus on psychiatric manifestations, with little to no emphasis on the metabolic and cardiovascular risk factors associated with PTSD. An emerging body of evidence shows that PTSD is a significant risk factor for metabolic dysfunction with higher rates of obesity, high cholesterol, high blood pressure, diabetes and heart disease. The precise mechanism by which PTSD increases the cardio-metabolic risk has not yet been determined, but emerging evidence suggests that the link between stress and metabolism is central. Stress, mediated through the sympathetic nervous system (“fight or flight”) and the hypothalamic-pituitary-adrenal (HPA) axis, leads to higher levels of the stress hormone cortisol. Chronically elevated cortisol levels result in abdominal obesity, which leads to insulin resistance and inflammation, the underlying processes that drive the risk of diabetes and heart disease. Cortisol also drives over-eating with increased consumption of comfort foods - high-calorie food choices. Compounding these effects of stress, people with PTSD show changes in brain function associated with appetite and changes in reward-processing that make the over-consumption of high reward foods even more likely. Our brain recognizes foods with these characteristics as innately rewarding:
Not surprisingly, research shows that individuals with PTSD have poor dietary habits and higher rates of emotional eating related to PTSD symptom severity. For some people with PTSD, the positive stress of exercise, with adrenaline release, increased heart and respiratory rates, can trigger PTSD symptoms. As a result, these people avoid exercise to minimize the risk of recurring effects of PTSD. The result is a more sedentary lifestyle that only further aggravates weight gain and poor metabolic health. Finally, the symptoms of PTSD often present with nightmares and disturbed sleep, further aggravating the stress response. The weight gain and metabolic changes increase the risk of developing sleep apnea, setting up another vicious cycle. How to address this? PTSD requires a comprehensive treatment plan, often combining counselling and medication. Often overlooked are the benefits of intensive lifestyle interventions to combat the effects of PTSD on diet, exercise, sleep and overall stress. Recognizing metabolic dysfunction, insulin resistance, pre-diabetes or diabetes and applying proven lifestyle approaches (like the 4+2 Diabetes Reversal Strategy) not only improve overall health but are synergistic to the primary therapy for PTSD. For RCMP: Wellness Garage offers a fully funded, comprehensive, year-long, multi-disciplinary lifestyle medicine program to help members with weight loss, nutrition, fitness and lifestyle optimization. The program is ideal for members with PTSD to pair with their psychological care plan. The program’s criteria are weight-based: BMI >30 or BMI 27-30 with a weight-related diagnosis. Although PTSD has not traditionally been thought of as such a weight-related process, the emerging evidence presented in the literature and reviewed here suggests that it should be recognized as such. Click here to learn more about this program. Even if you don’t qualify for the funded program - please reach out to have a Lifestyle Medicine Assessment (funded through MSP), where we can assess risk and help you develop a lifestyle strategy.  Photo by Kinga Cichewicz on Unsplash When it comes to your sleep, answer these four questions:
If your answers are yes to 1 and 2 and no to 3 and 4 - you do not have a sleep issue. You may be able to improve your sleep quality by falling the recommendations in 'How to Improve Your Sleep'…but feel fortunate and turn your efforts to one of the other pillars. You will notice that none of the questions here talk of time asleep or amount of deep sleep, REM, or any of the sleep scores you can derive from the variety of sleep trackers. If you sleep soundly and full of energy, you do not need to track your sleep. Even if you track your sleep - your answer to these questions is more important than any metric derived from a sleep tracker. If your answers are not optimal, you will want to improve your sleep habits while assessing yourself for sleep apnea or other sleep disorders. Use the Wellness Garage Sleep Checklist to assess your Sleep Hygiene and screen yourself for Sleep Apnea. Using a sleep tracker in this context can be very helpful to understand what actions you are taking that help or hinder your ability to sleep.
Finally, work with a Lifestyle Medicine physician or health coach to improve your sleep habits while addressing other practices that can improve sleep - especially exercise and stress tolerance. When you have tried everything to improve your sleep, but you are still not sleeping, it is time to dig deeper and determine if there is something else going on. By far, the most common sleep disorder is obstructive sleep apnea. It is estimated that up to 30% of Canadians suffer from it, yet only 6.4% have recognized the diagnosis. What is Obstructive Sleep Apnea? Sleep apnea is a serious condition in which a person’s breathing is repeatedly interrupted during the night. During normal sleep, air moves in an unobstructed, regular rhythm through the upper airway, the throat into and out of the lungs. With obstructive sleep apnea (OSA), airway blockages, usually from soft tissue collapse, prevent the normal regular breathing rhythm. What are the symptoms? The main symptoms of OSA are
However, some people have no symptoms or may not recognize that they have symptoms. Other symptoms may include one or more of the following:
The key to addressing sleep apnea is to recognize it - start with our downloadable checklist - if you score as high risk, talk to your doctor about getting a sleep assessment. (For more on Sleep Apnea - check out our previous post: Sleep Apnea - what you need to know). Other significant sleep disorders will get picked up through this review process. Excessive daytime sleepiness due to narcolepsy or other central types of hypersomnolence will be considered before or after sleep apnea is ruled out, depending on your history. Sleep-walking or excessive movements in bed, restless leg syndrome or other disorders are best managed with a referral to a sleep specialist. The Wellness Garage SLEEPSounder approach leverages a check-list system. Start by assessing your current sleep habits - we refer to this as sleep hygiene. In all cases, improving these will be part of the solution for your concerns. At the same time, screen yourself for obstructive sleep apnea - if you score anything other than Low - bring the checklist to your physician to review. They will determine the next steps - either a referral for a Home Sleep Apnea Test or a consultation with a sleep specialist. This was part 3 of our SLEEPSounder series, the other posts:
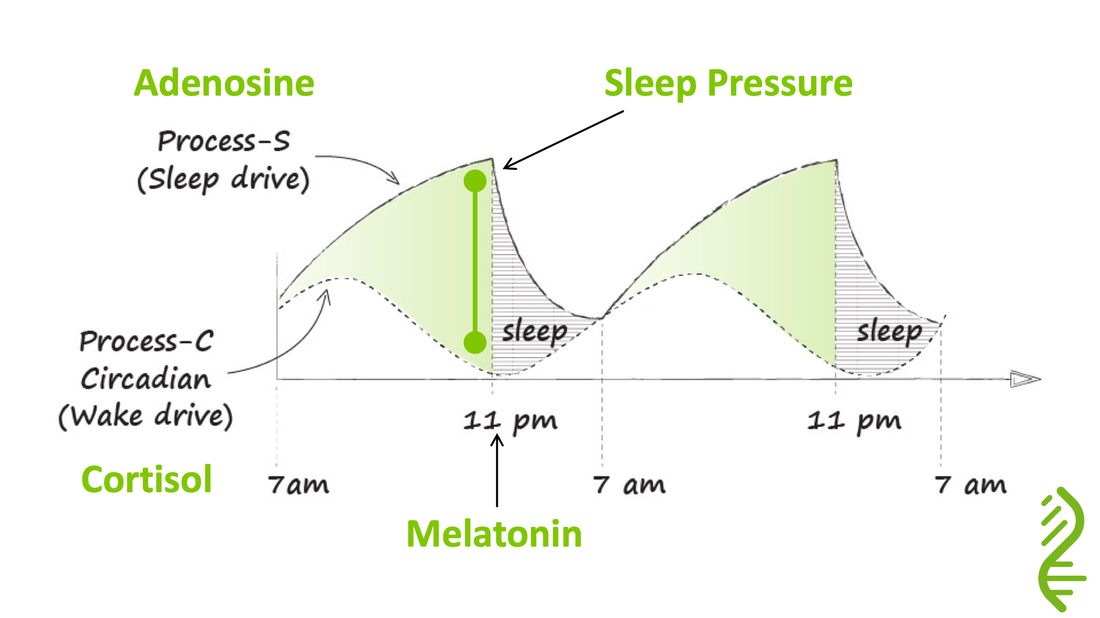
Getting a good night’s sleep is a challenge faced by many. Lack of sleep has become an epidemic in our society and is increasingly common as we age. There are many causes for poor sleep, some of which need medical assessment, but mostly our ability to sleep well is within our control. Here is a safe and proven framework for sleep. If you are not sleeping well after implementing this, a visit with your physician is warranted. A good night’s sleep is all about optimizing your behaviours and environment to fit your body’s natural rhythm. As humans, we have evolved to be awake when it is light and to sleep when dark. Supporting this circadian rhythm is a cascade of different hormones that signal the body to be alert or sleepy. Our days start with a morning burst of our ‘get up and go’ hormone cortisol, signalling that it is time to greet the day. Over the course of the day, our cortisol wanes until in the evening levels are close to zero. In parallel, adenosine levels build up, signalling fatigue. Adenosine is a by-product of energy expenditure – the more active we are, the greater our adenosine levels. Finally, when dark, our brains release melatonin signalling it is time to sleep. (read more about the Importance of Sleep) Aligning our behaviours to our body’s hormonal symphony is relatively straight-forward: First, avoid substances that will alter hormones and affect your sleep:
What do you do if this doesn’t work? If you have
Sleep Restructuring
This is the second part of our SLEEEPSounder series. Check out these other posts:
At Wellness Garage, we are here to support you in your health journey to take control of your health, restore confidence, and optimize your wellness. We do this through solid evidence-based medicine, personal health coaching and instruction, providing you with the knowledge, skills and support you need to apply healthy habits to your life. Learn more about how Wellness Garage can help you take control of your health. |
AuthorDr. Brendan Byrne Categories
All
|








 RSS Feed
RSS Feed
