|
“in order to keep well, one should simply avoid too much food, too little toil” - Hippocrates "The doctor of the future will give no medicine, but will interest his patients in the care of the human body, in diet, and in the cause and prevention of disease." - Thomas Edison The evolutionary process, from which modern humans arose, selected for traits optimized for an environment very different from what we live in today. Our hunter-gather forebearers, walked and ran long distances, often carrying significant weight. Hunger was a frequent companion, and they ate when, and as much as they could. Night-time was dark, a time for rest and sleep, daytime was active. By our standards, they were filthy - colonized by a diverse collection of bacteria, fungi and viruses. And though their microbiota were large and diverse their social groups were small - no greater than 150 people. Not surprisingly, evolution selected human genes that optimized our abilities to be calorie efficient and benefit from activity. We are designed to store excess calories in fat, to draw upon when calories are scarce, as they so often were. Our muscles and bones get stronger with usage. Our bodies operate on a diurnal rhythm with up to 30% of our genes turned on or off by the light-dark cycle, building in regular periods for cellular repair and regeneration. Many of our biological systems depend on interaction with a diverse variety of micro-organisms and their genetic products. Socially, our capabilities max out at around 150 relationships. So we find ourselves in an evolutionary mismatch between the world our genes were selected for and the sedentary, fast-food, 24 hour, constant stimulus, Facebook world. It is any wonder that the diseases we increasingly face at epidemic levels are rooted in this mismatch?
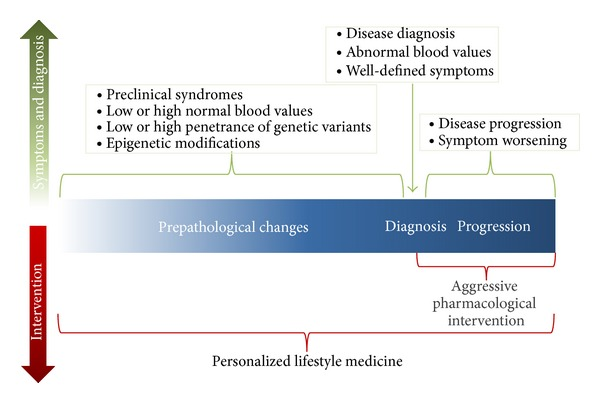
Simply put, we are not designed to live the modern lifestyle. Lifestyle medicine leverages this insight by utilizing lifestyle interventions such as nutrition, physical activity, stress reduction, sleep, smoking cessation and the avoidance of alcohol abuse to prevent, manage and reverse disease. This approach can be implemented at any point in a disease process, but it is important to realize that since most chronic diseases take 15 to 20 years to develop, environmental evolutionary mismatches slowly disrupt biological systems eventually cascading towards disease. These disruptions can be detected prior to the diagnosis of disease, and reversed through lifestyle behavioural interventions. Progress can be measured through improvements in key biomarkers. This strategy can be used alongside conventional medical approaches to help manage and actually even reverse disease. The most powerful examples of disease reversal come from Ornish’s (http://www.healthways.com/blog/the-future-of-health-care) work with heart disease and the recent application of therapeutic nutritional strategies for diabetes. It is no wonder that Lifestyle Medicine has been called "the Future of Healthcare”. At Wellness Garage, we use a lifestyle medicine approach to precisely assess our client’s current risk - we then help them develop lifestyle strategies to optimize their health and prevent disease. Where disease is present, we look to manage and reverse the underlying processes, often eliminating the need for medications. Our approach is evidence based and personalized to each client’s goals. To learn more - book a free consultation or request more information As many of you realize, I love the science of systems biology and really enjoy researching and explaining how things work in our amazing bodies. But as much as I enjoy sharing my wonder, I would never want people to think that health is something you need an MD or PhD to understand and optimize. Today’s post contains some really simple, actionable things that you can do every day - starting today. 1. Eat minimally processed foods Food is medicine - Food is poison. The simplest, and best place to start is by eating minimally processed foods - or as Michael Pollan would say - Eat Real Food. The evidence for this is overwhelming - processed foods (sugar, refined carbs, industrial vegetable oils, packaged goods with ingredients you cannot pronounce) are not good for you. Processed food:
…and you will feel better. While this sounds simpler than it actually is - it all starts with a decision to eat real foods, and to systematically avoid processed options, one choice at a time. In our coaching programs, we help people make these choices - starting with easy substitutions and building over time. 2. Sleep 7-8 hours of sleep - it does not get any simpler. Most people do not need more and very few of us can really get by on less. Many studies have shown clear links between inadequate sleep and poor health: increased inflammation, hypertension obesity, diabetes and heart disease. Adequate sleep also reduces improves sex, mood and thinking while reducing chronic pain, risk of injury or infection. …and it feels better to get a good night’s sleep. It all starts with a simple decision to prioritize sleep. At Wellness Garage, our coaches can help you create a sleep ritual that will work. 3. Move more Exercise is important, but it can take some work to develop an exercise routine that works for you. A simple first step - is to make a decision to move more. Get up often, walk more, take the stairs, park away from where you need to go - get off one subway station sooner than you need to. Think about moving - make the decision to be more active. Walk the dog - take a phone meeting while out walking - carry your groceries - do yard work - think of house work as exercise - anything that makes you use your body is good. …and you will feel better - this simple decision will lead you to want to do more, making it easier for you to build up your exercise practice. Our coaches can help you find the exercise routine that works for you. 4. Get Outside
The Japanese have a term Shinrin Yoku - which literally means “forest bathing”. The idea is to take a leisurely walk in nature, to take in the smell, the sounds, the feeling of being outside. This simple act of being mindful in nature has been shown to improve health by boosting immunity, lowering blood pressure, decreasing stress hormones and improving mood. …and it feels good. So go for a walk in your nearest park or woods, and bath in the atmosphere. 4. Spend more time with those you love For this, I am not going to cite any research but ask two questions:
Prioritizing relationships is good for your health and it feels good. Make the decision to do these five simple things, you will be healthier and you will feel better. Wellness Garage is a precision lifestyle medical practice, combining medical expertise with a team-based approach including one-to-one coaching, personal training, nutritional counselling, education and digital tracking. We provide comprehensive medical assessments of your health, using the latest, proven science, to help and support you:
To learn more - book a free consultation or request more information Today I am going to provide a list of 7 biomarkers for you health - numbers you should know. These are all biomarkers that can be improved through lifestyle interventions - they are numbers that can be normalized and optimized - and in doing so you will reduce your risk for heart disease, diabetes, cancer, Alzeimher's dementia, kidney failure, arthritis and many other conditions. Optimizing these biomarkers will even decrease your risk of premature death. I think this should be a pretty good investment of 15 minutes of reading! (If you want to skip the reading - there is a quick summary at the end of this post).
2. Gamma Glutamyl Transferase (GGT) - optimal < 30 U/L GGT measures a liver enzyme and is commonly described as liver function test most closely associated with the adverse effect of alcohol. GGT is however much more important as it is an indirect measure of the body’s glutathione supply. Glutathione protect cells against the oxidative stress resulting from metabolism. Without this protection the free radicals generated by mitochondria through normal metabolism with oxygen would accumulate, overwhelm and damage the mitochondria and the cell. In normal ageing it has been shown that it is this accumulation of oxidative stress that leads to many of the age-related diseases. In many ways, glutathione is consider the master antioxidant: working with as part of the enzyme glutathione peroxidase to protect membranes from oxidation, enabling Vitamin E and C in their anti-oxidant capacities as well as working directly. Glutathione is also a key component of the Phase II metabolism (detoxification) of drugs, hormones and xenobiotics where it works as a component of an enzyme Glutathione s-transferase (GST) that conjugates heavy metals, toxins and other compounds so that they become water soluble and can be excreted in the bile or urine. Exposure to high levels of toxins that overwhelm glutathione in its Phase II metabolic role will lead to oxidative stress. 3. hsCRP - high sensitivity CRP - optimal < 1.0 Again another topic I have recently blogged about: chronic inflammation. Chronic inflammation is at the root of 7 of the top 10 causes of death accounting for 80% of all deaths in our society. The most insidious aspect of this type of inflammation is its silent nature that allows for damage to occur without diagnosis. HsCRP is the gold standard for assessing chronic inflammation - optimizing this number through behavioural change - diet, exercise, stress reduction - decreases the risk for many diseases. 4. Blood Pressure - optimal <115/75 (systolic/diastolic pressures measured in mmHB) This is the simplest - something that you can do at home, at the local pharmacy and with your doctor. Normal blood pressure is 120/80. Recently there were major headlines in the US, noting a change in the definition of high blood pressure (hypertension), lowering the definition threshold to 130/80 from 140/90. While this change dramatically increases the number of people who will be diagnosed with hypertension - not all will automatically be recommended medications. Those recommendations will depend on a person’s overall risk for cardiovascular disease - anyone with a 10% or greater risk should aim to bring the BP below 130/80. High blood pressure or hypertension is quantitatively the most important modifiable risk factor for cardiovascular disease (the largest contributor to premature death in our society). It is also a significant risk factor for both kidney and heart failure. For every 20 mmHg increase in diastolic blood pressure above 75, the risk of death from heart disease or stroke doubles. Elevations in blood pressure are caused by dysfunctions within core biological systems
5. Fasting Blood Glucose and or HbA1c: optimal FBS <5.2mmol/L (normal <5.6 mmol/L); optimal HbA1c <5.0% Maintaining normal blood sugars is one of the most important and tightly regulated functions in your body. Diabetes mellitus (DM) is the condition when your body cannot maintain normal blood glucose levels. Type I DM is an autoimmune disease where the pancreas stops producing insulin. Type II DM, is characterized by insulin resistance, where the body no longer responds normally to insulin. In order to maintain blood sugars, the pancreas increases production of insulin - leading to elevated insulin levels which in turn trigger inflammatory changes, which in a vicious cycle further worsens insulin resistance. Insulin resistance precedes Type II Diabetes and can remain undetected for years, as glucose levels are maintain as normal until the pancreas begins to fail, which is relatively late in the process. Diabetes is diagnosed when FBS >7.0 or HbA1c >6.5% Type II DM is currently at epidemic levels globally having tripled since 2000. Almost 500M people or 1 in 11 have diabetes at an estimated cost of $850M. The direct complications from diabetes come from damage to blood vessels at two levels:
6. TG/HDL - Triglyceride/HDL ratio - optimal <1.0 Of all the information that can be derived from a lipid panel the TG/HDL ratio provides the best information about risk. TG/HDL is an excellent marker for insulin resistance and metabolic syndrome When elevated above 3.5 - this is the simplest test to identify atherogenic dyslipidemia, which is marked by the joint occurrence of elevated TG, low HDL and atherogenic, small, dense, LDL particles. This is highly predictive of cardiovascular disease. As we have seen above insulin resistance is the precursor to Type II DM and is often silent and undiagnosed, and is also one of the major causes of chronic inflammation. 7. Android:Gynecoid Fat Ratio - optimal <1.0 The major cause of the global diabetes epidemic is the associated obesity epidemic. Over 2B people are overweight with about 600M reaching the definition of obese (BMI >30). For obese people cardiovascular disease is the leading cause of death and disability, followed by diabetes. Kidney failure and cancer are the other major causes of death. Obesity, through adipocyte dysfunction leads to a chronic inflammatory state that predisposes an individual for many diseases. Abdominal or visceral fat contributes disproportionately to this inflammatory response as compared to peripheral fat. The best way to measure visceral fat is with a DXA body scan, which provides you with android:gynecoid fat ratio. The ratio correlates with insulin resistance, showing the clear link between visceral fat and the pathogenesis of diabetes. The added benefit of getting a DXA scan is getting understanding your lean muscle mass and bone density. As you age maintaining lean body mass and bone density are both essential for vital longevity avoiding age-related sarcopenia and osteoporosis. A good alternative (without the extra bone and lean body information) is a waist:hip ratio. The optimal ratio for men in <0.85 and women <0.75. Abdominal obesity is also a marker for metabolic syndrome - a cluster of conditions that carry risk individually but are collectively carry massive risk:
As you can see, all of the risks for metabolic syndrome have been covered by our 7 numbers.
According to a recent study - almost 1 in 5 Canadians, including 40% of people over 65 have metabolic syndrome . Unfortunately, many are unaware of it and have placed themselves at massively increased risk for diabetes, heart disease and premature death. In Summary - 7 Numbers You Should Know
Inflammation is the normal process by which the body responds to injury. When cells are damaged by trauma or infection, they send signals that mobilize the bodies immune system to understand and address the situation. The acute inflammatory response is recognizable by five cardinal signs: calor; rubor, dolor, tumor and functio laesa; if you have just twisted your ankle: it’s warm, red, painful, swollen, and you cannot use it. This response makes sense as it alerts you to your injury, and forces you to rest while facilitating the repair, turnover and adaptation of the injured tissues, or in the case of infection inflammation also prevents the spread of pathogens to nearby tissue. Without inflammation, we would not survive. Our challenge is that inflammation is meant to be an acute, self-limited process that facilitates healing. Chronic inflammation, unlike acute inflammation is a prolonged, maladaptive, low grade, persistent and dysregulated process that is the major contributor to chronic disease and ageing in our society. This silent but destructive nature makes inflammation a special challenge; by the time it is recognized, much of the damage has been done. Inflammation is implicated in 7 of the top 10 causes of death in Western societies accounting for over 80% of deaths. It is chronic inflammation that represents perhaps the biggest threat to our health and through the epidemic of chronic disease affects the sustainability of our health care systems.
So where does chronic inflammation come from?
The large variety of stimuli that fuel inflammation converge on a few basic mechanisms and pathways within cells - specifically the activation of the transcription factors NF-κB and Nlrp3 inflammasome which activate gene transcription and the production of inflammatory molecules called cytokines that interact with other cells to elicit a cascading response. This response leads to increased plasma levels of pro-inflammatory cytokines (Interleukin-6, IL-6, Interleukin-1, IL-1 and Tumour Necrosis Factor-α, TNF-α) as well as increases in the main inflammatory biomarkers such as C-Reactive protein (CRP) and serum amyloid A. This generalized pro-inflammatory state, interacts with genetic and environmental factors to potentially trigger the onset of inflammation-related diseases:
Given the multitude of triggers and profound potential consequences that chronic inflammation has, the logical question (if you have read this far) is: Am I inflamed? The standard test for this in the clinic is the high sensitivity C-reactive protein (hsCRP) - anything greater than 1.0 nmol/L suggests a low-grade inflammatory process, with levels greater than 3.0 nmol/L associated with elevated risk for heart disease (atherosclerosis). Levels greater than 10 nmol/L suggest an acute inflammatory response (infection). What is an optimal strategy to avoid inflammation? 1. Maintain optimal gut microbiota health and prevent leakage of gut microbes into the body
If you are having symptoms or have concerns about intestinal permeability - there are tests that we can do to determine whether leakage of microbes from your gut is contributing to your inflammation. Finally, if you are really interested you can check your microbiome and assess it's overall health - two caveats here: 1) there is huge variability between tests - these tests are really just snap-shots; and 2) there really is very limited data from these tests to direct you to a more specific response then I have outlined. 2. Minimize cellular damage from oxidative stress
4. Minimize the deleterious effects of high blood sugars and/or high insulin Our society is in the midst of a diabetes epidemic - it is estimated that between 50-70% of the population has been diagnosed with diabetes, elevated blood sugars (pre-diabetes) or elevated insulin levels (insulin resistance - the precursor to diabetes). While there are clear genetic risk factors, the overwhelming evidence points to lifestyle: poor diet - excessive nutrients of poor quality - high carbohydrate, high fat, combined with physical inactivity leads to elevated insulin levels which initially maintain blood sugar levels at the expense of increasing the storage of calories in fat. This increased fat storage leads to obesity with overloaded fat cells becoming dysfunctional and senescent and secrete pro-inflammatory cytokines which in turn cause insulin resistance - creating a vicious cycle. The inflammation eventually affects the pancreatic beta cells, decreasing their ability to secrete enough insulin to maintain blood sugars and a person is diagnosed as diabetic. The frightening part of this scenario is that it often takes 10-20 years to go from insulin resistance to diabetes - during that time levels of chronic inflammation increase as do the associated risks. For diabetes and insulin treatment and prevention the place to start is with diet as it is the most likely culprit. A whole food, low carbohydrate, healthy fat approach is the way to go. For diabetics on medication - ketogenic diets have an excellent track record as a therapeutic intervention to decrease or eliminate medications. As you can see from these strategies to avoid inflammation, the answer lies in your behaviours - especially eating, exercising, sleep and stress. Your optimal strategy will come from assessing and understanding your current situation and addressing your behaviours in a systematic fashion. If you are overweight (or simply over 40) you should, at a minimum, know your hsCRP, fasting blood sugar, HbA1c (3 month average of blood sugars), HDL cholesterol, LDL cholesterol, triglycerides and GGT (liver enzyme that also is a key marker of oxidative stress), as well as your waist to hip ratio. These are tests that every family doctor can (or probably has already) done for you - the important thing is for you to know. If any of these tests are abnormal (or not optimal), you should develop your own strategy to getting well. If these tests are normal, you should still review your core behaviours and assess what can still be improved. At Wellness Garage, we deliver comprehensive lifestyle medicine assessments reviewing all of this data, along with other optional tests that are not routinely offered in the publicly funded system: molecular data (genomics, metabolomics, proteomics, microbiome, and other advanced diagnostic tests), DXA scans (to assess body composition). We use all of this data to help you build the optimal strategy for your own personal wellness. We then can match you to a personal coach to help you implement the behavioural changes necessary. New Year’s Day is always a time for reflection, revaluation and resolutions. Often we take a look at our lives, see what is lacking and resolve to “fix” it…all at once. A flurry of activity, new gym memberships, calorie deficient diets and within 2-3 weeks we are back to where we started, Frustrated, we feel foolish to think that we could make the changes that we want in our lives. Today, as you reflect, I would urge you to do something simpler. Definitely take the time to reflect and reevaluate; understand where you are and where you want to be. Take the time to look at your core behaviours:
Instead of trying to “fix” everything, all at once, look for your good habits and try to build upon them, extend and expand them. Start with habits that you already have, tune and tweak them to be a bit healthier, and a bit more consistent. Give yourself time to incorporate these changes one or two at a time. Finally, make the time to reflect everyday, for a few moments at least, like it is New Year’s Day and realize that every day is a good day to be be a little bit healthier. At Wellness Garage, we believe in the power of habits, and that everyday is a good day to be healthy. We have launched our 2018 Healthiest Year Ever program, combining comprehensive lifestyle medicine assessments with personal coaching to help you find your healthy path. Check out the program here: https://www.wellnessgarage.ca/2018.html If you want to learn more, please book a free consultation with us. Happy New Year!! |
AuthorDr. Brendan Byrne Categories
All
|







 RSS Feed
RSS Feed
