Linked to the 24-hour light-dark cycle, humans wake at first light and go to sleep when dark. Along with sleep, much of our physiology is dependent on this circadian rhythm. 30-40% of our genes are either turned on or off by the presence or absence of light. So we have evolved to eat and be active during the day and to rest and digest at nighttime. But what exactly does sleep do? Increasing evidence points to the importance of sleep for brain maintenance. Our brains need downtime to clear the metabolic waste from the activity of thinking. During the day, our brains are highly active, with high metabolic demand. As the day progresses, metabolic waste increases and needs to be cleared for the brain to function optimally. When we sleep, glymphatic channels open in our brains, cerebrospinal fluid circulates, removing the accumulated metabolic waste. While this is happening, our neurons reshape themselves - building new synaptic connections and pruning old ones. Memories are consolidated from short-term storage in our hippocampus to long-term memory in our cortex. We learn new things at night when we sleep, and we forget things that are no longer important (like the number of the hotel room we just checked out of). Through our dreams, we also make new connections between different memories. Without sleep, these memory consolidations do not occur, and learning, memory, and psychological health all suffer. Without sleep, metabolic waste is not cleared, increasing the risk of dementia. Of course, the adverse effects of the lack of sleep go well beyond brain health:
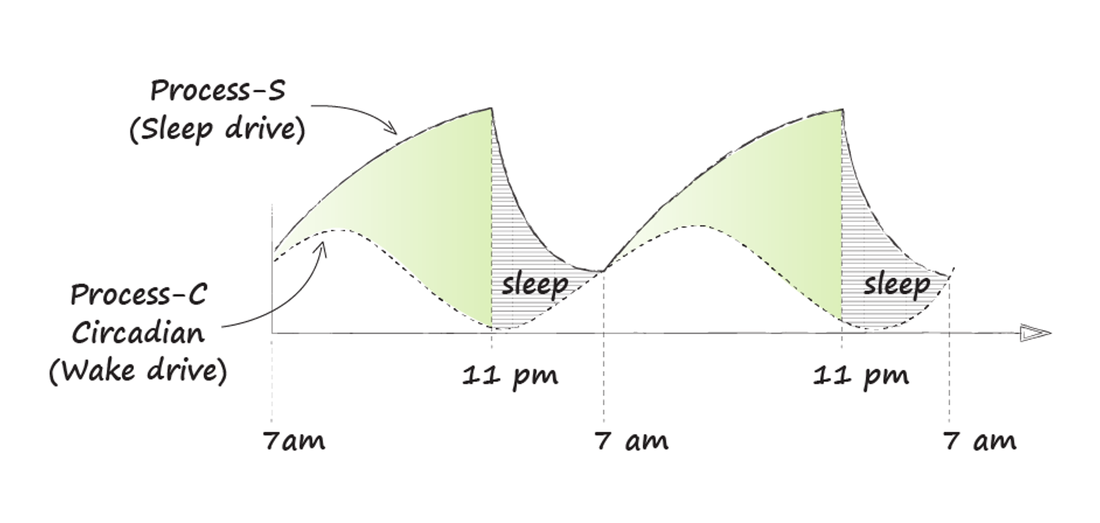
So while we may not fully understand all the effects of sleep, these associations remind us of sleep’s vital nature. Sleep architecture: When we sleep, our brains run through a predictable cycle of sleep stages: Light sleep: Stage 1 - transition from wakefulness to sleep Stage 2 - body temperature drops, heart rate slows, sleep spindles appear Deep sleep Stage 3 - muscles relax, blood pressure decreases, breathing slows Stage 4 - deepest sleep REM - (Rapid Eye Movement Sleep) - dreaming Each cycle takes approximately 90 minutes to complete. In the first part of the night, we get more deep sleep; in the second part, more REM. This pattern is likely related to the consolidation of memory in the first part of the night and new insights and creative connections in the second half. Even from this brief review, you can see the peril in cutting short your sleep. Losing 90 minutes of sleep may cut out a complete sleep cycle and, with it, the loss of learning and creativity. To understand how we can optimize our sleep, we need to know how sleep comes about. Sleep and arousal are closely tied to the light-dark cycle. In the early morning, just before dawn, our brains send signals to our adrenal glands to release cortisol. Cortisol, often referred to as our “stress hormone,” is really our “get up and go” hormone. It mobilizes energy and activates our brains and bodies to be alert for the day ahead. As the day runs its course, cortisol levels decrease until they are barely detectable in the evening before bedtime. As we are active, metabolites of brain activity accumulate, most notably adenosine. The subjective feeling of fatigue correlates closely with adenosine levels. In fact, caffeine blocks adenosine receptors and makes us feel more energetic by blocking the fatigue signal. The gap between the increasing levels of adenosine and the decreasing cortisol concentration has been referred to as sleep pressure. Throughout the evening, this sleep pressure builds until darkness hits and the pineal gland in the brain release melatonin, triggering sleep. How this sleep symphony of hormones plays out determines whether you have a good night of sleep or whether you lie in bed sleepless.
Aligning your behaviours with your sleep hormones is the best way to ensure that you get a good night’s sleep and all the benefits that accrue from it. The final post in the LEVELUp Your Fitness Strategy.
You now have learned the LEVELUp Your Fitness Strategy. How do I implement this? The first thing is to identify where you are starting from: If you have not been exercising regularly over the past month then start with steps 1 and 2: If you are exercising regularly (LEVEL 1), but not doing resistance training with adequate functional movement then start with steps 3 and 4: 3. Resistance training 4. Functional movement training Finally, if you doing all of this (LEVEL 2) but feeling plateaued in your fitness focus on: 5. Aerobic Progression For each progression, give yourself at least 6 weeks or longer. Seven keys to success:
What do I do if I get injured?
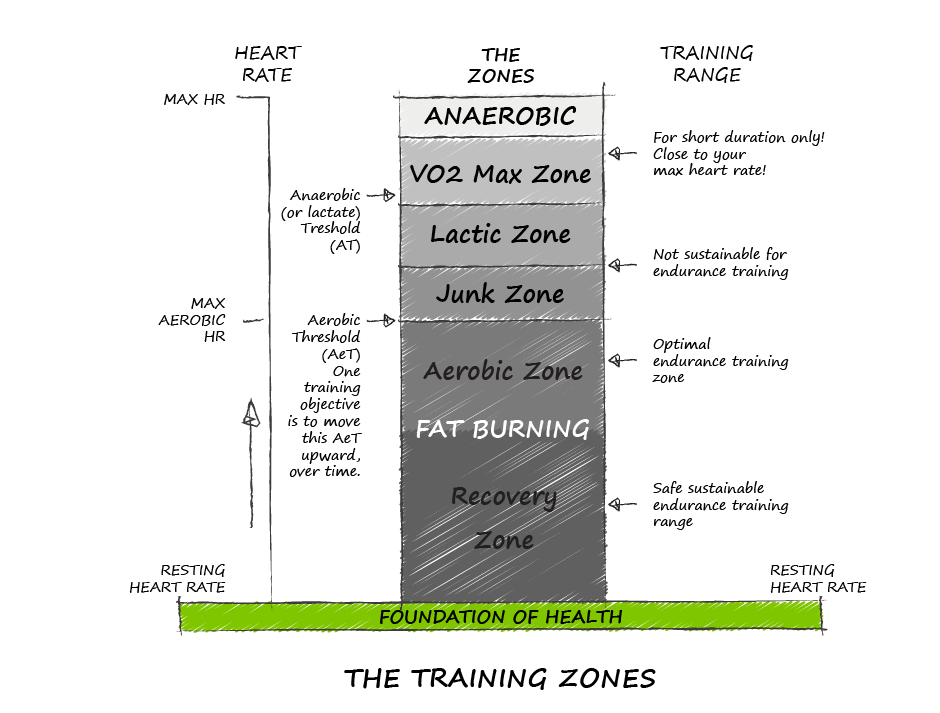
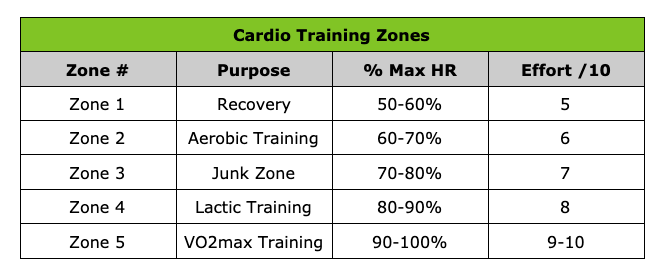
If you have pain that limits you from exercising for more than a few days, consult with a physiotherapist. It is much better to jump on injuries early than to wait. Your physio will be able to help you understand what to do to resolve the injury as well as (more importantly) what to do to prevent the injury from recurring. What if I miss a few days? Pick up right where you left off. Listen to your body and go more slowly if necessary. What if I miss a few weeks? Start back at 50-65% of your usual workload and duration. Focus on good form. Pay extra attention to warm-ups and stretching. Can I exercise if I have a medical condition? If you have a medical condition and are concerned about starting an exercise program, consult with your physician. The risks associated with following a well-designed exercise program are very low and the benefits far outweigh the overall risk. Need help? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. Your aerobic fitness progression eventually will take you to specific training types that develop the muscles’ energy systems. All force generated by muscle requires energy. All energy-requiring processes in the body use the energy stored in a molecule called adenosine triphosphate (ATP). ATP works like a battery storing a small amount of energy for future use. The metabolism of glucose and fat generates ATP, and muscles use ATP to generate the force that powers our activities. The more efficient you are at delivering ATP to muscles, the fitter you will become.  Photo by Tikkho Maciel on Unsplash Your muscles use three energy systems during exercise to provide ATP to generate the force required to meet the demands of your chosen activity. Although no system works completely independently from each other, one or a combination of two will become dominant depending on the exercise’s duration and intensity. Energy Systems 1) The Immediate System Muscles store a small amount of ATP that can be used immediately for a couple of seconds. Along with ATP, muscles also store something called phosphocreatine, which can rapidly generate ATP. This combination of ATP and phosphocreatine is known as the ‘immediate system.’ It is the dominant energy source during short durations (up to around 10-12 seconds) along with high-intensity efforts. Activities requiring short bursts of high energy: weight training, sprinting, and shot-put utilize the ‘immediate system.’ The availability of stored ATP and phosphocreatine becomes the limitation of the ‘immediate system.’ 2) The Glycolytic System For activities requiring high intensity for 30 seconds to 2 minutes, muscles use glycolysis, which rapidly converts glucose to lactate and does not require oxygen. After two minutes, the build-up of lactic acid becomes too high, and the muscles get that dreaded burning sensation and performance drops. Activities like hockey, CrossFit, and middle distance running and swimming (i.e. 800m run, 200m swim) predominantly leverage the anaerobic lactic system. The accumulation of lactic acid, rather than a fuel shortage (glycogen = stored glucose), limits this energy system. 3) The Aerobic Energy System Lower intensity activities utilize the slower aerobic system where glucose and fat combined with oxygen generate large amounts of ATP through oxidative phosphorylation in the mitochondria. Aerobic activity can be maintained for extended periods (hours). Activities like walking, jogging, running, hiking, cycling, biking, and swimming are predominantly aerobic. In the aerobic zone, your body will preferentially use fat for fuel, requiring oxygen to generate energy through oxidative phosphorylation. Your breathing will be more rapid than at rest, but you will not be gasping for air. Your heart rate will be less than 65% of your maximum heart rate. Above 65%, your body begins to recruit glucose (from stored glycogen) for energy. The aerobic system has no energy limitation as long as it is using fat. As you go faster, at intensities above 65% of maximal heart rate, your muscles will begin to use glucose from stored glycogen. Glycogen along will muscle fatigue are the ultimate limiting factors for the aerobic system. When you start exercising, we recommend that you spend most of your time in the aerobic zone. As your pace quickens and you have mobilized glucose from glycogen, glycolysis may not keep up with the slower, aerobic, oxidative phosphorylation and lactate levels will begin to build. The Aerobic Threshold is the point at which your energy is no longer provided exclusively from the aerobic energy system. Training at a pace slightly slower than your aerobic threshold is ideal for developing your aerobic system. (Zone 2 training.) As you develop the aerobic system, your pace will increase at the same intensity and heart rate, allowing you to go faster for longer before activating glycogen use (stored glucose). For long-distance athletes, the more efficient their aerobic system, the faster they will go at higher intensities. Even athletes in sports that do not predominantly use the aerobic system, like hockey or Cross-Fit, will find that improve aerobic endurance will increase their performance and improve their recovery. After you cross the aerobic threshold, lactate levels gradually increase until a point at which your ability to recycle lactate becomes overwhelmed, and lactate levels rise exponentially - this is the anaerobic threshold. At this point, you are no longer able to sustain a given workload, and fatigue sets in, which will limit your endurance ability. The anaerobic threshold is often a good predictor of endurance sports performance because athletes with higher thresholds can race faster for longer and at a higher percentage of their VO2max. You can train the lactic system, exercising at paces close to the anaerobic threshold. Training to Increase VO2max VO2max refers to the maximum volume of oxygen that your body can consume during exercise. Maximal oxygen uptake occurs at very high intensities of exercise. VO2max is a good measure of aerobic fitness. Workouts designed to improve VO2max are typically very high in intensity and only last up to a few minutes at a time. ZONE TRAINING Training zones are a way of quantifying specific intensities during your training. Heart rate or perceived effort can be great ways to determine your training zones; however, more specialized aerobic performance testing can allow you to determine the exact intensities for each zone. Each zone has a different training purpose. Zone 1 (Recovery Zone)
Zone 2 (Aerobic Zone)
Zone 3 (Junk Zone)
Zone 4 (Lactic Training Zone)
Zone 5 (VO2max Training)
For individuals looking to monitor intensity with heart rate training, identifying your maximum heart rate can be a great starting point. Here is an easy formula to estimate your maximum heart rate: Max Heart Rate = 220 - your age (For example, if you are 30 years old, your maximum heart rate would be close to 190 beats per minute (bpm) (220-30=190)). Progressing your aerobic capacity will require thoughtful combinations of workouts with different intensities. This type of training is best done with an experienced coach or exercise professional.
Need help with aerobic progression? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. So far in the LEVELUp Your Fitness Strategy, we have encouraged you to move, get 150 minutes of moderate to vigorous exercise, add some resistance training and functional movement to your routine. At this point, you are getting most of the benefits of exercise, and you are getting fit. Our next goal is to help you progress your aerobic fitness. Aerobic training or cardiovascular training (cardio) enhances muscular and cardiovascular endurance - you can do more for longer and recover more quickly. In other words, you have better energy to enjoy your life. Aerobic fitness also allows you to:
Our starting point for aerobic fitness is 150 minutes of moderate to vigorous activity maintained for 6-8 weeks. After this initial base, you are ready to think a bit more about aerobic or cardio workouts, starting with steady-state training. Steady-state workouts involve your major muscle groups (arms and legs) in continuous, rhythmic action. Walking, jogging, running, biking, swimming, hiking, rowing, using the elliptical or stair-climber - all lend themselves to steady-state cardio. The most important thing is to find something you enjoy! Start Low and Go Slow Your initial pace should be easy to moderate. You should be able to hold a conversation, though your sentences might be a bit clipped. Most importantly, you should feel fresh enough at the end that you could go longer. When you start or come back after some time off, this will feel really slow. Don’t worry; when you are consistent with your training, you will get faster at the same effort within weeks. The biggest mistake made at this point is to go too fast and get injured. Your endurance, fitness and benefits all build as you progress your steady-state cardio in duration, frequency and eventually intensity. The first progression we recommend is duration and frequency. When you start, you will likely be doing three 20-30 minute aerobic workouts in addition to your resistance training and functional movement. You will find that increasing the frequency of workouts and duration will go together. An important rule of thumb is to add no more than 10% volume to your load each week as you progress. For example, if you are jogging 20 minutes, three times a week, for a total of 60 minutes - 10% is only 6 minutes - that you will add to a single workout. As the volume builds, you will find it easier to add an additional workout. This initial phase of aerobic progression is often called ‘building the base.’ After several months, you will have the base necessary to progress to higher intensity workouts. Don’t rush this phase - at first, it will seem slow, but trust us, as you get fitter, you will get faster at the same intensity.  Photo by Martin Magnemyr on Unsplash Building to Higher Intensities Once you have a solid base of aerobic fitness, you can progress from easy to moderate paces to faster, more vigorous intensities. Training at higher intensities is an excellent way to improve your aerobic fitness but does have some potential drawbacks:
Higher intensity cardio is incredibly challenging and fatiguing for less fit individuals, hence the reason to take your time to build a solid base. The key to minimizing these risks is to plan carefully and listen to your body (or work with an exercise professional). Start with a single workout per week at a higher intensity. There are many different types of higher intensity workouts that you can add. Tempo Pace The simplest way to go is to increase the steady-state workout’s intensity to something called ‘Tempo Pace.’ Start with 5 minutes at your moderate conversational pace before accelerating to a speed that you cannot hold a conversation. Hold the faster pace for 20 minutes, then recover by finishing with 5 minutes at a slow and easy pace. HIIT (High-Intensity Interval Training) HIIT incorporates periods of intense, short-duration exercise with periods of recovery. These periods are referred to as the “work” interval and the “rest” interval. Work intervals are typically 3-5 minutes, although sometimes as short as 30 seconds, and they are performed at a vigorous intensity (6-8/10 effort). Rest intervals are often equal in duration to the work interval with a 1:1 ratio; however, shorter work intervals under 3 minutes typically require a 2-3 minute recovery. Usually, about 3-6 sets are performed. These intervals are best done with coaching and guidance as they are challenging to plan for as a beginner. Hill Workouts Using nature’s resistance, you can do interval training by doing intervals on hills. For example, you could do eight times a short, steep hill or four times a long, gradual hill. The key to hill training is to be sure that you can keep good form as you jog, run or bike up the hill. Fartlek Training The Swedish work “Fartlek” means “Speed Play” and is a type of workout that allows for moderate AND vigorous training. Typically easy pace training is performed for most of the workout with brief high-intensity intervals scattered throughout. It can be performed in a structured or freestyle manner and is a great way to improve both the aerobic (low intensity) and lactic (high intensity) energy systems. Fartlek training is also a great way to keep workouts fun, and is often used in running, cycling, and swimming. An example of Fartlek Training is going for an easy jog but then sprinting up each hill you come across. Besides increasing your steady-state cardio intensity, you can add high-intensity training to your week by combining these workouts with your resistance training. Circuit Training Resistance training can be a great way to push the aerobic system as well. Performing various rounds of exercise combinations at vigorous efforts can be an efficient way to hit strength and cardio in the same session. Circuit Training is sometimes referred to as HIIT training as well, as periods of recovery may be incorporated, or intervals of different exercises are performed. Here are some of the many examples of circuit training: Superset Training Superset training involves performing two exercises back and forth rather than resting after 1 exercise. For example: Perform the bench press for ten reps, then instead of resting performing the bent-over row for ten reps. Repeat for the desired number of sets and rest as needed. Classic Circuit Training Classic circuit training involves performing various exercises (typically 3-4) without rest in a round. For example, bench press for ten reps, bent-over row for ten reps, squats for ten reps, repeat and rest as needed. Tabata Choose an exercise that you will work with for a total of 4 minutes in duration. Perform the exercise for 20 seconds, get as many good-quality reps as possible, and rest for 10 seconds. Repeat this for eight sets (4 minutes). EMOM (Every Minute On the Minute) Perform the given exercise for the prescribed number of reps for a minute. If you finish early, rest for the rest of the minute. If you don’t finish, move on. Start the next set over again once the new minute starts. Other exercises can be integrated into an EMOM workout. SAMPLE EMOM: 6 minutes of 10 burpees and a 45-second plank Minute 1: 10 burpees Minute 2: 45-second plank Minute 3: 10 burpees Minute 4: 45-second plank Minute 5: 10 burpees Minute 6: 45-second plank Be sure to follow every high-intensity training day with an easy day - steady-state cardio or functional movement. Never do two hard workouts back to back on consecutive days. For most non-athletes, regular folks, two hard workouts per week is enough. Listen to your body and progress slowly to avoid injury and burnout; if you are fatigued on your hard-workout day, just perform a lighter one. Burning Fat? Performing aerobic exercise causes your body to break down either glucose, fats, or both for energy. Since glucose is broken down rapidly, higher-intensity efforts rely mostly on glucose over fats rather than lower-intensity efforts, which typically rely on a combination of the two. Teaching the body to rely on fats Base training or light training (especially in a fasted state) can help the body learn to rely on fat oxidation: the breakdown of fatty acids for energy. This is done by training at lower (moderate) intensities at a steady pace. Providing glucose by eating carbohydrates pre-workout will force the body to use the glucose for fuel since it is the most available energy source. Because of this, fasting before this type of training is encouraged. If fasting is not possible, make sure not to eat too many carbohydrates immediately before or during exercise. Relying on fats for energy is excellent for sparing muscle glycogen (stored glucose). This can, in turn, help to prevent hunger cravings post-workout and allow an individual to exercise for long periods. For long-distance endurance athletes, training to improve fat utilization is essential to not run out of glycogen at the end of their race. Running out of glycogen causes a steep drop in energy - a truly awful feeling known as “hitting the wall.” Need help starting resistance training?
Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. Next Week - Technical Notes on Aerobic Progression Our next area to review in the LEVELUp Your Fitness Strategy is Functional Movement. Functional movements are movements based on real-world situational biomechanics. They usually involve multi-planar, multi-joint movements which place a demand on the body's core musculature and innervation.” - Wikipedia In other words, functional movement refers to the ability to move well for the required tasks. What is considered “functional” depends on the task your want to perform. Typically athletic movements like squatting, running, pushing and pulling are all considered functional, but specific movements should be prioritized for different individuals and sports. For example, pulling movements for rock climbing, balance movements for seniors, and agility movements for soccer players. Training to increase functional movement will improve athleticism and the ability to control your body through space. Functional movement training should be incorporated into your week of physical activity and improved or maintained through sports, resistance exercise, balance drills, agility training, and much more. Since everyone needs different areas of focus, your functional movement training should be unique. How do I know if I have good functional movement? Here are some of the factors that contribute to good functional movement:
If you feel that you lack these areas, your functional movement could probably use some work! Aim to identify your weak spots and progressively improve them through practice and training. Identifying your weak points can be challenging, so here are a few simple tests we use at Wellness Garage that can help to assess your functional movement.
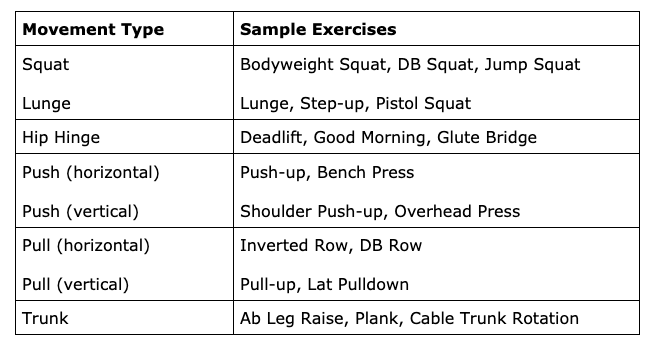
These are all movements that you can improve with training. If you feel that you need help assessing and improving your functional movement, seek advice from an exercise specialist. Injuries If you have a recurring or current injury, correctly rehabbing it will be essential to improving and sustaining high-quality movement long-term. Proper warm-ups and prehab strategies can also maximize injury prevention. Are weight machines functional? Although many people consider weight machine training to be “non-functional,” it would be a shame for bodybuilders and other muscle-building athletes to avoid them! Since machines typically do not demand the same level of stability and technique that free weights do, they allow us to push the muscles harder with good form, often targeting muscles in a way that free weights cannot. Machines can also be great for new gym-goers or people with physical limitations. While machines don’t improve athleticism and body coordination to the same degree as free weights and bodyweight exercises, there is a time and a place for them.  Photo by Sergio Pedemonte on Unsplash Functional Resistance Training Working out can be a great way to improve functional movement. Here are the primary movement patterns in resistance training that will improve strength and athleticism while hitting all of the major muscle groups:
Functional Resistance Reference Chart Most comprehensive workout programs designed to increase muscular strength and athleticism should include these fundamental movement patterns. These movements should generally be prioritized and performed before machine and isolation exercises (i.e. bicep curls, leg extensions, pec flyes).
Other Functional Movements Other types of athletic training, such as plyometrics and agility training (i.e. jumps, hops, skips, leaps, bounds, shuttle runs), are also very functional; however, they are more advanced and require a greater focus on technique. Make sure you have a base in strength training and technique before attempting these types of workouts. Plyometric and agility training should always be performed first in the workout before the body becomes fatigued. What if I can’t perform one of these movement patterns? If you have a restriction (mobility, injury, etc.) and cannot perform one of these movement patterns, work around it by hitting the same muscles with alternative exercises. For example, train the shoulder muscles with DB Front Raises and DB Lateral Raises instead of Shoulder Presses. See an exercise specialist if you need help with this. Neuromuscular Training Neuromuscular training to improve balance, stability, coordination, and proprioception (kinesthetic sense) is essential for maintaining athleticism and quality of life. This type of training is critical as we age, as it can improve activities of daily living and prevent falls and other injuries. Specific neuromuscular exercises like balance and agility drills are typically performed at the beginning of a workout (right after the warm-up) while the mind and body are still fresh. Performing at least 60 minutes per week of neuromuscular exercise is most effective in improving athleticism and is typically performed in bouts of at least 20-30 minutes. Some examples of balance and agility drills include:
Stretching Stretching is a great way to improve and maintain the range of motion at a joint and is often a significant area of focus for individuals looking to improve their movement quality. If you have tight muscles or movement inhibited by a lack of flexibility, consistent stretching can correct this issue. Several types of stretching increase movement quality and range of motion Static Stretching
Dynamic Stretching
Ballistic Stretching
PNF Stretching (proprioceptive neuromuscular facilitation)
Foam Rolling (and other manual release techniques)
For most people, static stretching (passive) is the recommended method for safely increasing range of motion long-term. Stretching Guidelines
How long does it take to increase range of motion? While individual results vary, typically, you will see results after four weeks of consistent stretching (2-3 times per week). If you do not see results in this time frame, try increasing your weekly stretching time or speak with an exercise professional. When should I perform my stretching? You can stretch any time of day; however, optimal movement comes by increasing the muscles’ temperature beforehand. Try 3-5 minutes of light aerobic activity or use external heating sources like a hot pad or a warm bath to warm muscle. Don’t do static stretching in your warm-up. Static stretching (roughly >30-45 seconds) immediately before exercise can reduce the ability to generate strength, power, and sports performance, so for this reason, avoid static stretching until after your workout. If you want to increase your movement quality and range of motion without decreasing your performance, try dynamic stretching and foam rolling. These are much better options for your warm-up! Stretching Program We have created a sample general stretching plan for increasing range of motion - click here for the details. Warming Up Warming up increases exercise performance and reduces the risk of injury by circulating blood to the active muscles, preparing the body for specific movements, increasing mobility, and improving muscle activation and proprioception. Here are some different types of warm-ups that everyone should incorporate into their exercise. 1) General Warm-Up A general warm-up improves circulation, increases blood flow to the muscles, moderately raises your heart rate, causes you to sweat slightly, and gets your mind ready to start exercising. General warm-ups usually take about 5-10 minutes and are often performed as light cardio. 2) Dynamic Movement Warm-Up Dynamic movement warm-ups are often the most neglected type of warm-up but are very important. A proper dynamic warm-up typically includes short duration stretches and functional movements that will allow you to feel more limber and stable before exercise. Some dynamic warm-ups are used for injury management and muscle activation as well. Dynamic movement warm-ups can take anywhere between 5 and 20 minutes, depending on how well you are moving that day. Generally speaking, if your movements feel restricted and less stable than usual, prolong your warm-up. Examples of dynamic warm-ups are leg swings, inchworms, lunge and twists, and hops. 3) Exercise-Specific Warm-Up Don’t work too hard, too soon! Working up to your maximum output for the day is essential for injury prevention and performance. Slowly working up in weight or speed allows your muscles and nervous system to start acclimating to the stimulus. The first thing to do in an exercise-specific warm-up is to make sure you groove the movement. Grooving a movement means practicing it until it feels proficient enough to start increasing intensity (i.e. warming up with the bar before squats, light jogging before sprinting, etc.). Once the movement is grooved, spend a few minutes working up to your full intensity for the day. Warm-up Program We have created a sample warm-up you can use before workouts - click here for the details. Need help starting resistance training? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. Next Week: Progressing Aerobic Fitness Last week, we outlined a strategy to add resistance training to your fitness plan so that you can maximize the health benefits of exercise. This week, we add some Tips to guide you as well as some sample workouts to get you started. Remember, if you need personalized support consider doing a TARGET Fitness Plan TIPS for Resistance Training Treat each set as though it’s the only set of the day. Perform as many good quality reps as possible for each set you do, and don’t worry about how many sets you have left. Progression Progress by adding resistance (weight, band tension, or increase the rep range for bodyweight exercises) once you can exceed your rep range (i.e. 15 reps) on any of your sets. Variance on reps The rep range is a guideline, and sometimes you’ll be slightly above or below. That’s ok! For example, if your program calls for 3 sets of 10-15 reps, you may perform 14, 10, and then only 7 reps because your muscles have become fatigued. Don’t worry about it! If you complete less than 6, consider lowering the resistance. Tempo In weight training, take 1 second to lift the weight and 2-3 seconds to lower it back down. We encourage this tempo as a baseline to help master technique, improve stability, keep good tension on the muscles, and prevent the risk of injury from an uncontrolled movement. If you aren’t weight training, treat whatever type of resistance you are using in the same way (i.e. pull the band in 1 second and lower it in 2-3 seconds). Breathing Breathe out on the exertion phase (i.e. lifting the weight) and in on the recovery phase (i.e. lowering the weight down) Mind Muscle Connection Make sure you can feel the muscles you are trying to work. Start with a warm-up Warming up is essential because it can improve performance and reduce the risk of injury. Start with 5-10 minutes of light aerobic activity (such as steady cycling or walking) and then perform a few dynamic stretches like 10 arm swings and 10 leg swings. More advanced warm-ups are encouraged later on, but this is a great start. How much weight to use? Use a weight that causes you to achieve failure (or close) roughly within your rep range—getting the right weight often takes some trial and error. When to change it up? Change it up if you aren’t progressing or if you are getting bored. However, it is good to spend at least a few weeks on the same program to give your body time to progress your exercises. Track your progress Make sure you write down the date, how much resistance you used, and how many reps you performed. This way, you know if you’re progressing and when to increase your resistance. Some pain is good! Resistance training is not easy, and it requires a little bit of pain tolerance, but it has to be the right kind of pain. When you lift, your muscles will start to feel a burning sensation as they temporarily accumulate with lactic acid and other metabolites. This feeling is normal during resistance training and should start subsiding shortly after completing your set. In addition to this, your muscles may swell up a little during training - this is normal and occurs from increased blood flow. Another sensation you may experience is delayed onset muscle soreness (or DOMS) due to acute inflammation. The body attempts to heal the microtears in the muscles acquired through strenuous training. If you have DOMS, you will feel pain or stiffness in the muscles when you contract, move, or stretch them. DOMS doesn’t always occur after training and usually occurs less as you become more adapted to your workouts. Some pain is not good! Pain in the joints or sharp pain in your muscles is a concern both if it occurs suddenly or after exercise. If this happens or you are unsure whether exercise is safe for you, consult with your doctor or an exercise professional. Although resistance training is typically relatively safe, training with poor technique or weights that are too heavy for you can result in pain and injury. Good form is critical Although it is important to train hard, it is more important to learn how to perform each exercise correctly with a full range of motion (ROM) to stay safe and maximize your training. Ensure you have good form for every rep, and get professional instruction from an exercise professional if necessary. Always learn proper technique before pushing yourself on an exercise. If you can’t meet with an exercise professional, there are many excellent YouTube channels with videos on exercise techniques. Here are a few of these resources:
High reps with relatively light weight High reps and low reps can both be beneficial for improving muscular strength and hypertrophy (muscle growth), according to a study in 2010 by Stuart Phillips at McMaster University in Hamilton, Ontario. As muscles approach failure, more muscle fibres are recruited to help overcome the resistance. This recruitment response is why lighter weights can be used to drive similar strength and hypertrophy adaptations to heavier weights (which recruit more muscle fibres straight away). It should be noted that training to failure is still challenging and that training to failure with high reps (i.e. 20 or 30) may be more challenging for some people than training with a more traditional number of reps (around 10) because the set takes longer to perform and metabolites continue to accumulate in the muscles. Don’t overthink it! A 2020 study published at the Federal University of São Carlos in Brazil compared three different training programs amongst a group of 60-70 year old adults. One group trained to failure, one group just shy of failure, and one group with a fixed amount of reps (10 reps). The fixed rep group did less than a third of the failure group’s total work, yet all groups had similar increases in strength and functional performance (walking speed and getting out of a chair). When you are starting resistance training, the bottom line is that showing up to do the workout matters more than the degree of effort and numbers of reps. Although trained lifters need to push themselves to drive adaptation, newer lifters can get away with just performing the exercises with reasonable effort. Next Steps
Workout Programs See our selection of beginner workout programs for those with different levels of fitness and equipment availability. We recommend these full-body workouts 2-3 times per week with at least one day of recovery in between sessions. Need help starting resistance training?
Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. NEXT Week - Functional Movement Once you have mastered LEVEL ONE of our LEVELUp Your Fitness Strategy:
The improved cardio-respiratory fitness you will get from mastering LEVEL ONE has many benefits, including increased longevity (low cardio-respiratory fitness is associated with twice the incidence of all-cause mortality). However, an independent factor, muscular strength (along with mass), provides an increased longevity boost of a similar magnitude. Muscular fitness also improves:
So to get the full complement of benefits from exercise, we recommend that you LEVELUp by:
Resistance training is any exercise where your muscles resist external forces. This external resistance can come from your body weight, weights (barbells, dumbbells), machines, bands, or anything heavy! The goal is to improve muscular fitness by increasing:
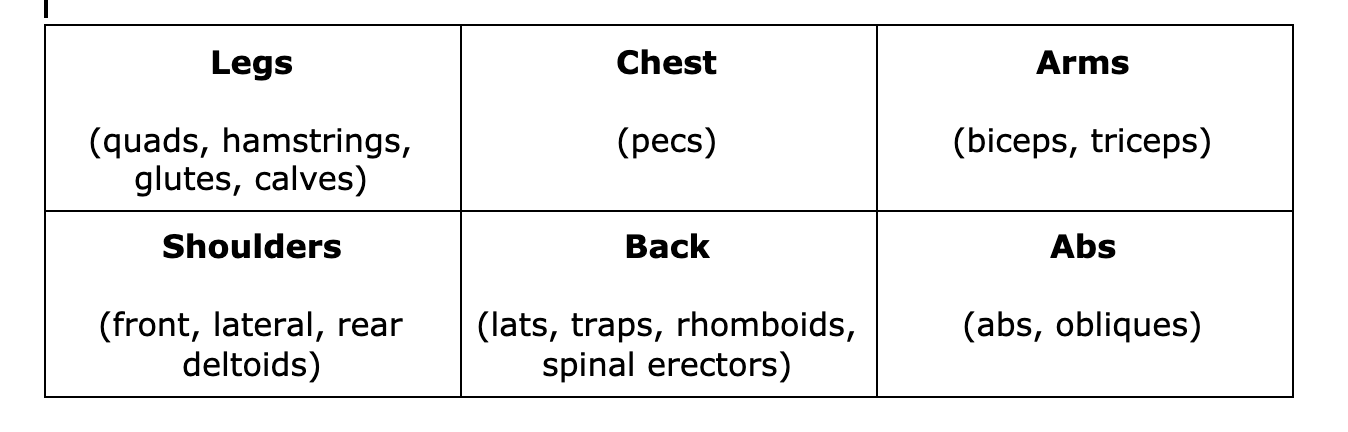
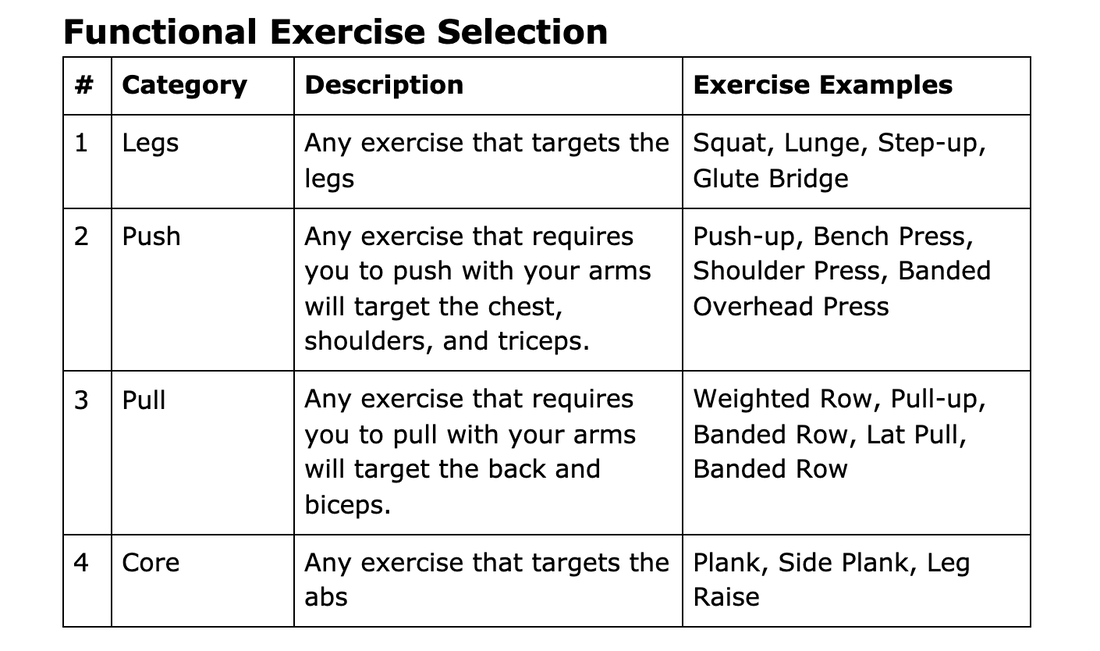
For beginners, this means either two full-body workouts - for more advanced programs, this could represent multiple split-body workouts each week. What are the six major muscle groups? Which exercises hit the major muscle groups? There is a limitless supply of exercises to choose from for resistance training, and it can be challenging for beginners to prioritize specific exercises over others. Choosing the exercises for your workout can be simplified by focusing on four major categories of exercises. A functional full-body workout includes at least one exercise from each of these four categories. These four categories will cover the major muscle groups. If you are creating your workout, choose four exercises, one from each category! Here is an example of a weight training workout that incorporates an exercise from each of the four categories: 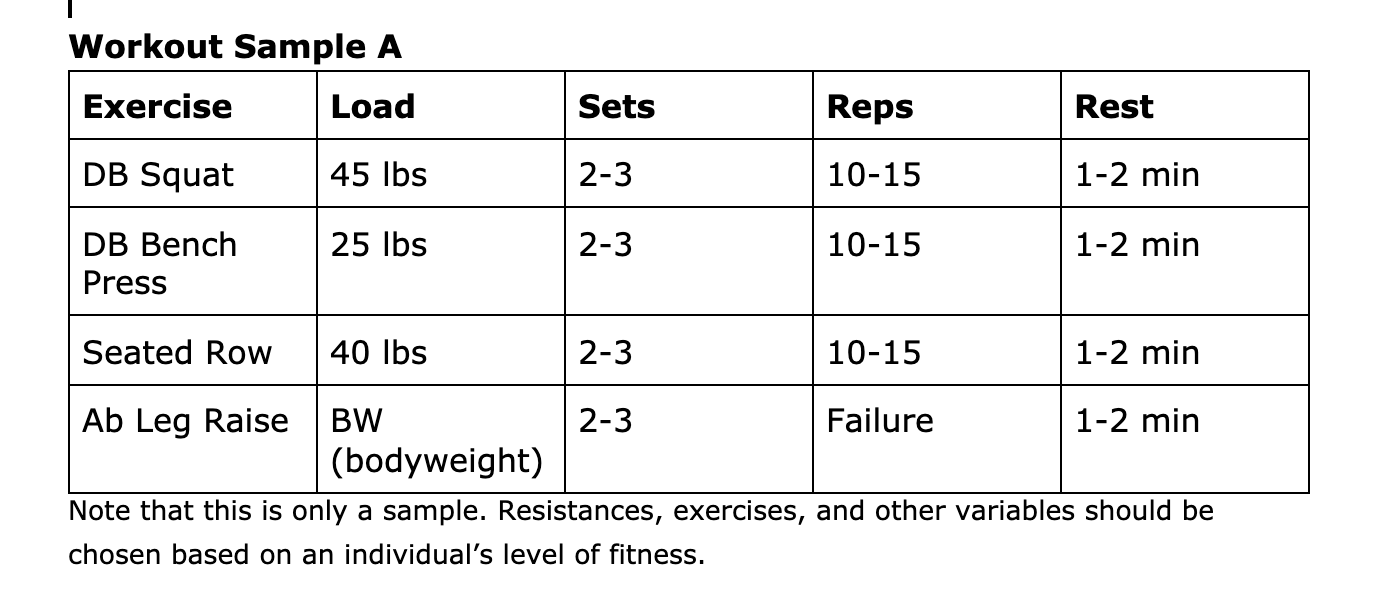 Variables for Resistance Training Reps (repetitions) How many times you perform an exercise in a row (i.e. 10 squats). Sets How many times you perform a group of reps (i.e. 2 sets of 10 squats). Perform all sets of a given exercise before moving on to the next. Resistance How much resistance you use (i.e. a load of 20 lbs, a red resistance band pulled back 1 meter away, your body weight). Rest How long to take a break before repeating another set of the given exercise (i.e. 1-minute rest between sets of push-ups). Recovery Recovery is the process of allowing the body to recover from the training stimulus. Muscles are damaged slightly during resistance training and take about 48 hours to recover and get stronger, making sure not to train the same muscles hard every day. Getting proper sleep, nutrition, and taking time off of hard training is essential to maximize recovery. Training to Failure Training to failure means performing as many reps as possible of a given exercise until the muscles can no longer produce enough force to overcome the resistance or until the proper technique starts to break down. Perform most exercises within a few reps of failure (about 0-4) to ensure the muscles are challenged enough to drive adaptation. Guidelines for the Workout There are many ways to train, but we recommend that beginners utilize the following guidelines:
Need help starting resistance training? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. NEXT Week - Part 2 - Tips on Resistance Training Exercising for 150 minutes or more per week at moderate to vigorous intensity will provide you with most of the health benefits of exercise. Multiple sessions, as short as ten minutes, add up to keep you fit and healthy. Combining exercise with moving throughout the day while avoiding long periods of sitting provides a strong foundation for a healthy life.  Photo by Lital Levy on Unsplash In our LEVELUp system, we refer to this as: Level 1
Remember, consistency is much more important than intensity. When you consistently hit these targets for 6-8 weeks, you will be ready to progress to Level 2. What is moderate to vigorous physical activity? Intensity depends on your fitness level. Your breathing will be an excellent guide. During moderate-intensity exercise, you will be breathing more rapidly than at rest, but you can still have a conversation, although your sentences will be a little shorter as you catch your breath. At vigorous intensity, holding a conversation becomes more difficult or impossible! Some examples of moderate-intensity:
150 minutes sounds like a lot of time!
Spreading out your exercise across six days maximizes the benefits while only taking 2% of our waking hours. We recommend at least three days per week of exercise. The challenge when you start is that the individual session may seem long if you exercise fewer days. Either way - make a plan that works for you. We also recommend that everyone at this level take at least one day off per week from exercise. A day off will keep you fresh. Of course, you will need to stay active and move throughout your off-day. How do I know when to increase the duration of exercise? Go slow and listen to your body. Moderate exercise should feel relatively easy and should leave you feeling refreshed and energized. You should not be fatigued the following day. If you feel fatigued at any point as you build up, decrease the duration for a few days until the fatigue passes, then build by adding a few minutes every few days. Decreasing the duration is always better than taking the day completely off. Let fatigue be your guide. If I haven’t exercised previously (or in a long time), what should I do? For most people getting started, walking will be the first mode of exercise. Walking is simple, low-risk, and accessible to most people, and moving briskly or going up hills can be a great way to elevate the heart rate. If walking is not accessible to you, consider swimming, cycling, or using an exercise machine (i.e. stationary bike, rowing machine, elliptical, etc.). What if I’m ready to push myself? Wait until you have been exercising for at least four weeks before you push yourself. This will give you a base of fitness that will prepare you for higher intensity. It will also decrease your risk of injury. After four weeks, you can increase your intensity in a workout and see how your body responds. Every few weeks, you can add another vigorous-intensity workout until you reach three per week. Always follow a vigorous (hard) day with a moderate (easy) day. If you are fatigued on the day you have scheduled your vigorous workout, go with another moderate (easy) day. Listen to your body and progress slowly. Walk before you jog, jog before you run, run before you sprint. Injuries are common when intensities become too high too quickly. You should always start with lighter efforts and gradually increase the effort as your body feels healthy and ready. Remember, now is the time to build excellent behaviour patterns and a strong aerobic base. The time for intensity will come later. Making the Change Developing consistent exercise behaviours is key to mastering Level 1. Here are some tips to help keep you consistent:
Once you are up to 150 minutes per week, keep it up for 6-8 weeks, and you will have mastered Level 1! We hope that you can keep the Level 1 behaviours indefinitely, but we encourage you to take the next step and move to Level 2. More exercise will generally provide more significant benefits, and incorporating Level 2 behaviours certainly will. Asking for Help If you are experiencing any of the following, consider meeting with your doctor, physiotherapist, or an exercise professional like a kinesiologist or exercise physiologist to help you on your exercise journey:
Final Plan We will use the FITT principle (frequency, intensity, type, time) to highlight our plan to master Level 1. F - Move every hour, exercise daily. I - Moderate to vigorous intensity. T - Steady aerobic exercise. T - Move breaks for 2-5 minutes, exercise for 20-25 minutes. Good luck mastering Level 1! If you need help changing your behaviours, Wellness Garage is here for you. Need help applying this to your busy life? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. The first step to an active lifestyle is to move throughout the day. Exercise protects against chronic disease and premature death. Conversely being sedentary, increases the risk against these same diseases and is itself associated with premature death. It has been estimated that prolonged sitting is responsible for 3.8% of deaths and that every hour of sitting is as harmful as the benefit from twenty minutes of exercise. A recent meta-study of over 1 million people demonstrated that it takes large volumes (60-75 minutes per day) of moderate to vigorous exercise to offset the risk of prolonged sitting. Even at this level of activity, some risk remains. The highest risk group is people who spend more than eight waking hours sitting and do not exercise. The lowest risk group spend less than 4 hours being sedentary and exercise 150 minutes or more per week. Prolonged sitting carries increased risk for both men and women across
Simply put, prolonged sitting is very damaging to your health and cannot be offset by exercising alone. Unfortunately, sedentary behaviour is an epidemic in modern life. In Canada, a review across all occupations showed that all workers spent a high proportion (65% to 73%) of their day being sedentary. How is all this sitting damaging our health? There are at least three mechanisms that drive the health risk of being sedentary:
A striking demonstration of how quickly this happens was a Danish study where healthy young men were instructed to limit their daily steps to less than 1500 per day. After just two weeks, they developed:
Combatting this sedentary behaviour through regular intervals of physical activity can significantly reduce these risks and provide health benefits. A multi-year analysis of 4757 people demonstrated that breaking up sitting with short breaks decreased waist circumference, reduced inflammation marker and improved blood glucose. Sitting is not the only sedentary behaviour! While we have focused on sitting, remember that lying and reclining are also sedentary behaviours. Even standing is better - studies show that it uses about 8-10% more energy than sitting. Moving every hour for a few minutes is optimal to gain the health benefits from exercise. Make sure to develop a few strategies that you can implement to increase your physical activity throughout the day. What are some ways that I can incorporate movement into my busy life?
Doing errands:
Start by choosing one or two behaviours that resonate with you, or perhaps create your own. Aim to increase your heart rate/breathing and muscle activity for 2-5 minutes every hour. Making the Change It takes effort to implement a new behaviour, and it will not happen unless you plan for it. Take a moment and consider where, when, and how you will implement this physical activity into your day. Consider the barriers to these behaviours and how you will accommodate or overcome them. Sample Scenario You are planning to walk around your floor three times every hour at work. Barrier 1: Getting busy with work and being “in the zone,” forgetting about it Solution 1: Setting an alarm or timer for every hour and putting the break in your schedule Barrier 2: Getting caught in a long, sedentary meeting Solution 2: Walking during potential breaks, pacing around the room or standing if possible, making sure to move before and after the meeting Planning for success is an essential step in changing your behaviours, and setting SMART goals is critical. Sometimes I just don’t have time. The reality is, you will have time to be healthy if you make time to be healthy. At moments (especially at work), tasks can be overwhelming, and time can feel restricted. Often the last thing you want to do when this happens is get up and move because you just want to finish up what you’re doing. Taking a 2-minute break from 58 minutes of steady work is not a huge time commitment. This short break is almost certainly going to improve your performance of the task, as physical activity is an excellent avenue for mental clarity. If you have found that breaks and distractions have impeded your productivity in the past, perhaps physical activity breaks will have a different effect. If not right away, then give it some time. Your body will get used to it and will thank you in the long run. Moving throughout the day is the vital first step of living a healthy and active lifestyle. If you need help changing your behaviours, Wellness Garage is here for you. Need help applying this to your busy life? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy.
These benefits combine to improve longevity, reducing premature death from all causes by 16% and from cardiovascular disease by about 25%. Looked at another way, lack of physical activity is estimated to be the 4th leading cause of death and the principal cause for approximately:
These benefits come from relatively minimal efforts: 20 minutes of exercise and the avoidance of prolonged sitting every day. Twenty minutes a day to feel better and live longer - not a bad trade-off! The World Health Organization has set 150 minutes of moderate to vigorous activity/exercise and the avoidance of prolonged sitting (>8 hrs per day) as the threshold required to get most of the benefits from physical activity. Of course, the benefits do not stop at 150 minutes, and many people feel better with two, three or four times that amount. Not everyone incorporates consistent physical activity into their week, and these guidelines can be intimidating for those with busy schedules or a lack of exercise experience. In fact, only 17% of Canadians get 150 minutes of “moderate-to-vigorous physical activity” per week. (2019 Canadian Health Measures Survey) This strategy will get you started and help you progress. Master each principle before working on the next. If you are new to exercise, start at the beginning. If you currently exercise, review each principle and begin with the lowest one you are not yet doing.
By following this strategy, you will develop habits that incorporate aerobic, resistance and functional movement activities, allowing you to accrue the benefits of exercise sustainably forever. We categorize exercise behaviours into two levels and encourage mastery at Level 1 to maximize physical activity enjoyment while minimizing injury. Level 1 At this level, you meet the WHO standard and accrue most of the health benefits from exercise.
After 6-8 weeks of consistently hitting these targets, you have mastered Level 1. You will have the foundation to progress your exercise to the next level, getting even more benefit in the process. Level 2 This next level expands on the foundational behaviours by incorporating a portfolio resistance, aerobic, and functional movement training into your routine.
After 6-8 weeks of consistently hitting these targets, you have mastered Level 2. We hope that everyone can become Level 2 athletes, progressing their fitness and enjoying the benefits for the rest of their lives. Next week: Move throughout the day - the first step to an active lifestyle. Need help applying this to your busy life? Get a personalized fitness plan to help you get started, progress or improve your enjoyment of physical activity The TARGET Fitness Plan gives you expert advice to transform your exercise habits - whether you are getting started or want to improve your current program. Our exercise physiologist will assess what you are currently doing and provide you with a personalized fitness plan based on the LEVEL Up Your Fitness Strategy. |
AuthorDr. Brendan Byrne Categories
All
|





















 RSS Feed
RSS Feed
