|
It's that time of year again in Canada, days are short and still getting shorter, light is fleeting and we are talking about Vitamin D. In this post, I am going to answer the questions we get about Vitamin D:
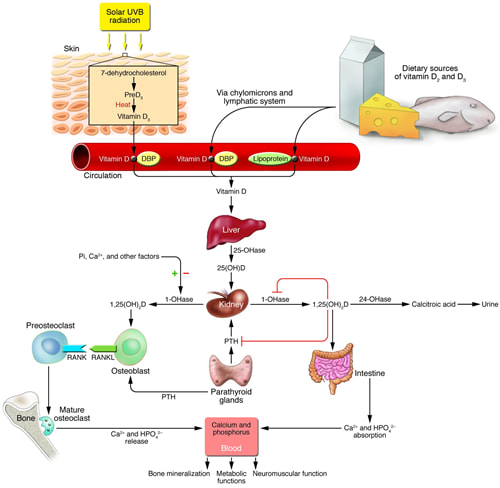
Vitamin D, the “sunshine vitamin", is a powerful hormone that your body makes through exposure to sunlight. From an evolutionary perspective Vitamin D is one of the oldest hormones found in biology, first appearing over 500 million years ago as a cellular factor protecting proteins, DNA and RNA from UV light damage. As organisms ventured from the oceans to land, a mechanism to obtain adequate calcium was necessary to maintain vertebrate skeletons. Calcium is abundant in oceans but on land, it is locked in soil and only available to plants. Vitamin D, synthesized in response to sunlight, evolved to ensure the intestinal absorption of calcium. For many years, this was what we understood about Vitamin D: that it is essential for proper calcium metabolism and bone health. Deficiencies in Vitamin D leads to rickets, the childhood disease of bone weakness, bowed femurs and tibias. Supplementing with dietary sources of Vitamin D to prevent rickets goes back to the early 1800’s with the use of cod liver oil (high in Vitamin D) and became mainstream in the 1930’s when milk was fortified with Vitamin D. Vitamin D Physiology Vitamin D3 (cholecalciferol) the hormone precursor is synthesized from 7-dehydrocholesterol in the skin in response to ultraviolet B (UVB) rays. UVB rays are present only during midday at higher latitudes and do not penetrate clouds. The time needed to produce adequate vitamin D from the skin depends on the strength of the UVB rays, the length of time spent in the sun, and the amount of pigment in the skin. At our northern latitude, UVB strength is not adequate from October to March so we must supplement. Very few foods naturally contain significant amounts of vitamin D (fish, shiitake mushrooms being exceptions) so obtaining adequate Vitamin D from non fortified food alone is difficult. Even with food fortification, it is thought that most Canadians have insufficient Vitamin D levels for optimal health. From production in the skin, Vitamin D binding protein transports Vitamin D3 to the liver where it undergoes hydroxylation to 25(OH)D - the half-life of this Vitamin D pro-hormone in the liver is 3 weeks. 25(OH) D is transported from the liver to the kidney where it is hydroxylated by 1 alpha hydroxylase (CYP27B1) to 1,25(OH) 2 D - the active form of Vitamin D. Both 25(OH)D and 1,25 (OH) 2 D are degraded by 24-hydroxlase (CYP24A1). Vitamin D then acts on the intestine to increase the absorption of calcium, on the bone to increase bone resorption and increase blood levels of calcium and on the kidney to decrease calcium and phosphate excretion. Vitamin D’s role in calcium physiology is clear and several meta-analyses have shown that supplementation with Vitamin D and calcium decrease the risk of osteoporotic fractures in older people. More recent research has shown that Vitamin D regulates many other cellular functions:
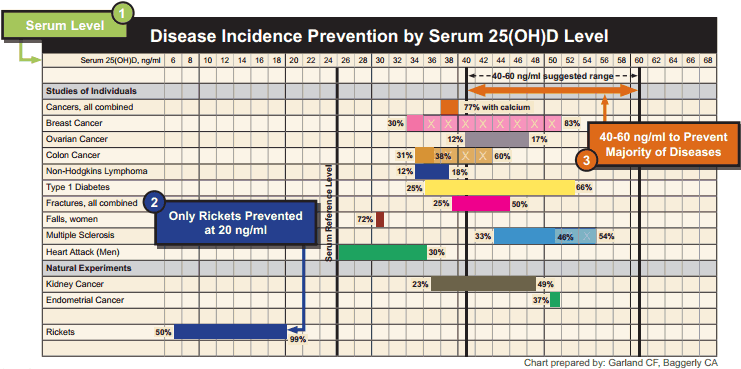
An explosion of research has suggested the Vitamin D may prevent or be useful in treating more than 100 disorders, ranging from:
All this evidence makes one thing clear - blood levels of Vitamin D are a good indicator of health across many conditions; what is less clear is whether low levels of Vitamin D cause poor health outcomes or whether the poor outcomes themselves can decreases in Vitamin D. The only way to determine this is through well designed double-blind supplementation trials, which are expensive and difficult to do properly. Still for many of these conditions trials are underway to determine the potential causal role of Vitamin D in many conditions. There are many factors that lead to signifiant variation in blood levels of Vitamin D:
So at this point we have established:
So the next question is how much Vitamin D should I take? This is where things get a bit controversial. If we look at disease association data, the optimal Vitamin D 25(OH)D blood levels appears to be between 100 - 150 nmol/L (40-60 ng/ml) The venerable Institute of Medicine (IOM) stated in their 2010 guidelines that levels of 50 nmol/L ( 20 ng/ml) are adequate. At Wellness Garage, we are most comfortable when clients are in the 100 - 150 nmol/L (40-60 ng/ml) and recognize that levels of >200 nmol/L (80ng/ml) are potentially toxic. So how much Vitamin D do you have to take to reach this level? Again this is controversial… The IOM bumped its recommended dietary intake from 400 to 600 IU for adults and for 800 IU for age >70 years. The maximum level was set at 4000 IU. Many, including us at Wellness Garage, think these recommendations are low. For those who have not been tested for Vitamin D, we recommend 2000 IU per day. For anyone taking doses greater than 5000 IU we also recommend testing. For those who can afford testing, we recommend getting tested during the winter December to February and adjusting your supplementation based on the results. Vitamin D testing is no longer a medically insured service in most parts of Canada due to the cost, especially when a simple one size fits all recommendation to supplement will likely help most people. We think this makes sense from a public policy perspective, at least until there is better evidence to support that supplementation itself prevents or reverses disease. We do think that individuals who are looking to optimize their health should test as there are simply too many variables to ensure that a standard dose of Vitamin D will put you in the optimal zone AND we feel that while the causal role of Vitamin D has not been proven for most conditions, it is one of the most important health indicators and the potential benefit of optimizing Vitamin D levels outweigh the negligible risks with supplementation when guided by testing. So if you skipped over most of this to find the answers to your questions - here is a quick summary:
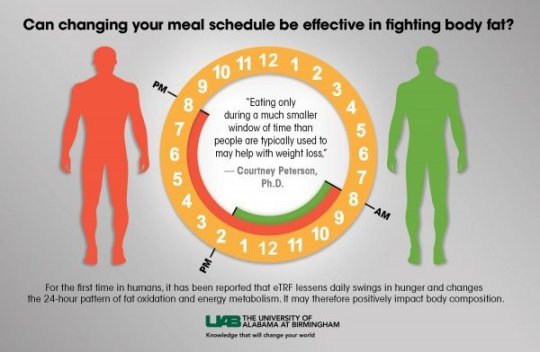
“Eat like a king in the morning, a prince at noon, and a peasant at dinner.” Maimonides (1135–1204), a medieval Jewish philosopher/doctor After eliminating refined carbohydrates from your eating, the next food recommendation we give clients looking to optimize their health and longevity is “time restricted eating”. What does this mean? Time restricted eating is a form of Intermittent Fasting (IF) where you eat all of your calories within a defined interval of time - generally 8 to 12 hours. This simple habit, has profound impact, likely due to two related evolutionary mechanisms:
To really understand why let’s step into the science. Life has evolved under the strong influence of the light and dark cycle. The predictable, 24 hour, diurnal rhythm has led evolution to develop internal timing mechanisms known as circadian (from the Latin words, circa diem, about a day) rhythms that are foundational to our biological systems. Fundamental to these rhythms is the ability to acquire food when it is available, and utilize the derived energy throughout the rest of the day, without impairing the organism’s fitness and vitality. A wide array of physiological and metabolic variations depend on the time of the day, including:
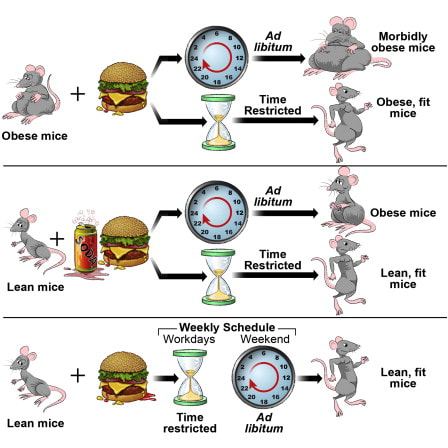
The past two decades have witnessed a remarkable increase in our knowledge of how circadian biology is controlled, both from physiological and molecular standpoints. Briefly, circadian rhythms are controlled by a master or “central” clock that is located in the hypothalamus within a paired structure known as the suprachiasmatic nucleus (SCN). The SCN oscillates on a 24hr rhythm independent of external input, but can be reset (or upset) in response to external cues. The SCN synchronizes other peripheral clocks which are thought to exist in all tissues in order to coordinate physiological processes. The clock adapts to environmental changes, specifically daily light-dark cycles, as well as rhythmic food intake. Nutritional challenges reprogram the clock, while time-specific food intake has been shown to have profound consequences on physiology. Elucidating the molecular mechanisms by which circadian rhythm is controlled earned Jeffrey C. Hall, Michael Rosebush and Michael W. Young the 2017 Nobel Prize in Medicine. Their work describes how specific transcription factors CLOCK and BMAL1 regulate the transcription of a large number of clock-controlled genes throughout the body in tissue-specific patterns allowing for the circadian regulation of cellular, metabolic, and physiological functions. A large fraction (30-40%) of the human genome appears to be under clock control. Studies of human metabolism shows that ∼15% of all identified metabolites oscillate in a circadian manner. Both food and light are powerful controllers that can reset (or upset) the circadian rhythm. Limiting feeding to less than 12 hours per day, a practice known as time restricted eating has been shown to protect against obesity, hyperinsulinemia, hepatic steatosis, and inflammation even when subjects are eating high fat, high carbohydrate, poor quality diets. These positive effects continue even after subjects stop time restriction and hold when applied only 5 days per week. The biggest caveat to this research at this point is that most of the evidence comes from mice, human studies have been indirect and correlative. Clearly more work needs to be done. With time restricted eating, one component of the benefit clearly comes from alignment with baseline circadian physiology - the other comes from the benefits of fasting. The fasting period serves as a period of repair and restoration with a set of certain biological processes that are only triggered in a fasting state known as fasting physiology. From an evolutionary perspective, the ability to survive periods of starvation makes sense. Starting from simple celled organisms, cells reprogram themselves during periods of fasting. The mechanisms of fasting physiology are evolutionarily preserved and present in all organisms. Inducing fasting physiology not only enables survival but also extends lifespan and does so in a preserved fashion with common mechanisms from single cell organisms to rodents. Reduced energy intake, or caloric restriction (CR), is known to extend life-span and to retard age-related health decline in a myriad of species, including nonhuman primates. Studies in obese patients show that CR can significantly decrease weight while improving cardiovascular risk factors, insulin sensitivity, and mitochondrial function. Two major challenges emerge from CR, one - it is very hard to sustain; and two - when sustained it results in decreased lean muscle and loss of strength which is of course not ideal for vital longevity. Efforts to gain the benefits of CR in a sustainable manner have led to the increasing popularity of intermittent fasting (IF). IF can take many forms but essentially involves fasting for periods of 12 hours or longer:
IF regimens have been shown to:
One key to these beneficial effects appears to be the “flipping” the metabolic switch:
This shift happens through a myriad of intracellular regulators including AMPK, mTOR and FOXO1 and results in cells cleaning up damaged intracellular proteins and organelles such as mitochondria. This self-cleaning process called autophagy is one of the most important functions of fasting physiology associated with anti-ageing and longevity. We know that oxidative stress and inflammation suppress autophagy, and suppressed autophagy leads to cellular inflammation and oxidative stress - a vicious cycle linked to both ageing and cancer. Our lifestyles, starting with the presence of artificial light allow us to be active throughout the full 24 hour day. Combined with the abundance of food, it is not uncommon for many people to consume some calories throughout every waking hour. Finally given the chronic sleep deprivation, endemic in our societies, many people may only be in a fasted state 6 hours or less. The challenge for these people is two fold:
At Wellness Garage we work with our clients to build habits that align with the natural processes of the body: circadian rhythms and fasting physiology in order to optimize health. For most people implementing these simple habits is simple, having profoundly positive effects (with little to no downside):
|
AuthorDr. Brendan Byrne Categories
All
|


 RSS Feed
RSS Feed
