|
Last week, we detailed the process of insulin resistance and how Type II Diabetes develops. Diabetes is a disease of sustained energy overload that develops over many years. The body’s normal energy buffers gradually become overwhelmed, and stored energy in the form of fat disrupts the normal function of key organs. This disruption through a process called insulin resistance, creates a vicious cycle where energy once stored cannot be accessed, and the energy overload is perpetuated through hunger and increased appetite. Eventually, fat stored in the pancreas overwhelms the body’s ability to maintain normal blood sugars and the diagnosis of diabetes is made. On average it takes 10 to 15 years for this process to unfold. So the logical question arises - can we reverse this process? The short answer is yes. The first line of evidence for this comes from bariatric surgery, where as long ago as 1992 studies showed that between 30 and 70% of diabetes can be reversed for over 10 years. In more recent years, Dr. Susan Hallberg and her team at Virta Health, have shown reversal of diabetes through a dietary therapeutic intervention. Their results with a ketogenic diet, show that 60% of diabetics are in remission at the end of one year. Impressively, the population consisted of many individuals with longstanding diabetes as well as many taking insulin. Of those, 94% decreased dosage or eliminated insulin entirely by one year. From my perspective the most powerful research has come out of the UK from Dr. Roy Taylor and his colleagues in Newcastle. Through a series of clinical trials, culminating in the DIRECT study. They systematically showed that insulin resistance correlates and is caused by fat in the liver in the liver, and the development of abnormal blood sugars and diabetes correlates and is caused by fat in the pancreas. Eliminating the fat in the pancreas can restore the body’s ability to release enough insulin after eating and eliminating the fat in the liver restores the body’s ability to maintain normal fasting blood sugars. So how much fat do you need to lose in order to reverse diabetes? If you had a magic wand and could eliminate fat directly from the pancreas and liver you would only need to eliminate less than 1 pound - as it is estimated that the amount of excess fat in the liver is approximately 400g with even less ectopic fat in the pancreas. Taylor’s group estimates that even as much as 1ml or 0.6g of fat reduction from the pancreas is enough to restore pancreatic insulin secretion in patients that respond to weight loss. Of course, the challenge is that we do not have a magic wand so we must seek to lose weight and trust that some of it will come from the fat stored in our liver and pancreas that is causing our insulin resistance and diabetes. The DIRECT study was a randomized clinical trial (the highest source of clinical information) that demonstrated that 86% of patients that lost at least 15kg were able to put their diabetes into remission. The therapeutic intervention was a hypocaloric diet (830 calories per day) provided by meal replacements. Further research by Taylor has shown that patients that subsequently slipped back into diabetes regained pancreatic fat. Common to all three lines of evidence, the degree of diabetes reversal correlates directly with the amount of weight lost. So the evidence is clear that diabetes can be reversed provided you can lose enough weight and keep it off. It’s that last bit - and keep it off that is problematic. The challenge with using a diet to lose this weight is that diets do not work over the long term. Temporary restrictive approaches - whether it be of calories (DIRECT study) or carbohydrates (VIRTA Health) are prone to regression. The only way to get long term results is through a behavioral approach. Change habits in order to achieve sustainability. The 4+2 Diabetes Reversal Strategy is built on this behavioral change model, incorporating an understanding of the physiology of insulin resistance and Type II Diabetes.
Step 1: Eat to Lower Insulin Decrease insulin requirements by decreasing the intake of simple and refined carbohydrates. Replacing refined foods with whole foods with a special focus on fibre will result in less insulin required to maintain blood sugars. Pairing fibre rich, low glycemic, whole food carbohydrates with adequate protein and healthy fats helps normalize blood sugars after meals and provide steady glucose supply from food for hours. Step 2: Use Your Muscles Recognizing the role of skeletal muscle as the key energy buffer for glucose; the next part of the 4+2 Diabetes Reversal Strategy is to leverage exercise and activity to increase the uptake of glucose from meals into muscle. This uptake in turn decreases the amount of glucose converted to fat by the liver. Step 3: Be Kind to the Liver The ability to maintain blood sugars while fasting is dependent on the liver making glucose from glycogen or other sources (gluconeogenesis). Fat in the liver causes insulin resistance and results in the liver over-producing glucose with a corresponding elevation in fasting blood sugar. Decreasing fat in the liver is necessary to reverse diabetes, therefore decreasing fructose and alcohol - two substances that are directly metabolized into fat in the liver is essential. In addition, focusing on gut health with adequate fibre intake has been shown to improve liver function. Step 4: Restore Fat Burning The first three steps create conditions that improve metabolic flexibility and allow the body to burn fat, but at the end of the day ‘less calories in, than calories out’ is necessary to lose weight. One of the most effective behavioral approaches to weight loss is time restricted eating starting at 12 hour of fasting and increasing to 14 to 16 hours as tolerated. Time restricted eating works because it eliminates nighttime snacking and results in fewer calories consumed making a deficit more likely. It also improves metabolic flexibility and the use of fat as fuel when fasting. When this is done after the first three steps, it is generally very easy to incorporate with minimal hunger symptoms. The +2 in the Diabetes Reversal Strategy involves decreasing the negative effects of cortisol on insulin sensitivity. Step 5: De-stress Finding ways to bring down cortisol without resorting to calories improves our ability to lose weight. Techniques as varied as meditating, yoga, time in nature and pursuing your hobbies have been shown to dissipate stress and bring cortisol levels down. Step 6: Improve Sleep Inadequate sleep elevates cortisol and appetite, often driving poor food choices (ie. comfort foods high in both fat and simple carbohydrates). Studies clearly show that adequate sleep can reset our stress mechanisms resulting in lower cortisol levels and improve appetite control. The 4+2 Diabetes Reversal Strategy works at the behavioral level to gradually and systematically shift to new healthy habits that are sustainable for the long run. Over time, blood sugars are better controlled, medications are reduced, weight is lost and diabetes is reversed. There is no magic to this - just sound evidence-based behaviours supported by science. At Wellness Garage we have developed a number of programs to support people who want to take control of their health and reverse diabetes: Our 4+2 Diabetes Reversal Group sessions are MSP funded group medical visits designed to provide you with all the information you need. Our 1:1 Coaching Program provides you with individualized nutrition, exercise and health coaching support to guide you to your own reversal path. “How did you go bankrupt?” Bill asked. “Two ways,” Mike said. “Gradually and then suddenly.” Ernest Hemingway, “The Sun Also Rises" Like Hemingway’s description of bankruptcy, Type II Diabetes develops gradually and then suddenly. Diabetes is a disease of sustained energy overload that develops over many years. The body’s normal energy buffers gradually become overwhelmed, and stored energy in the form of fat disrupts the normal function of key organs. This disruption through a process called insulin resistance, creates a vicious cycle where energy once stored cannot be accessed, and the energy overload is perpetuated through hunger and increased appetite. Eventually, fat stored in the pancreas overwhelms the body’s ability to maintain normal blood sugars and the diagnosis of diabetes is made. On average it takes 10 to 15 years for this process to unfold. To understand diabetes we need to understand how our body is designed to manage energy. Energy comes from food. Specifically the fats, carbohydrates and proteins that make up the food we eat. Our bodies have two different and related ways to store energy from food: glucose and fat. Glucose is the preferred fuel for our brains and converts to energy faster in our muscles, but it has two major limitations:
Our brain’s consume 1 tsp of glucose per hour and at rest the rest of the body consumes 1 tsp per hour. In other words, our blood glucose is turned over twice per hour. This glucose is supplied directly from food when we are eating and absorbing meals and from stored glucose (glycogen) when we are fasting. Our livers can only store about 150g of glycogen - for perspective this represents only 15 hrs of basal glucose production (150g = 30 tsp = 15 tsp @ 2 tsp/hr). Fortunately our livers can also make glucose from fat, protein and lactate (broken down from muscle glycogen). So our livers are constantly trying to maintain blood sugar levels by either breaking down glycogen (glycogenolysis) into glucose or breaking other compounds (gluconeogenesis). These processes are both controlled by the pancreas through the release of two hormones:
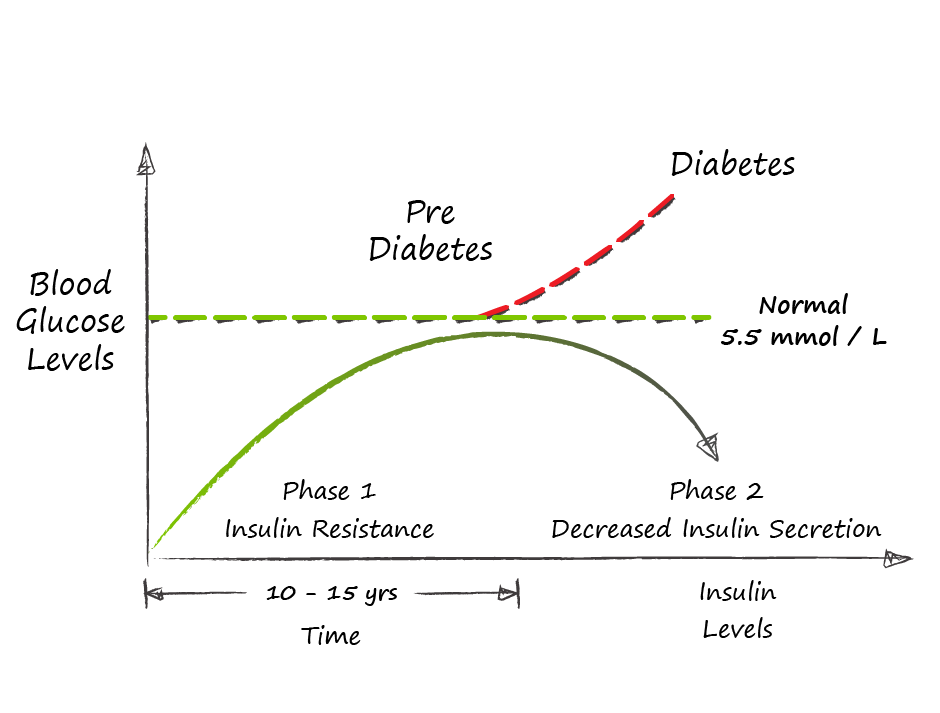
Fat is our slow fuel and we have unlimited capacity for storage. Each gram of fat has 9 calories vs the 4 calories in a gram of glucose and fat can be stored as triglycerides (3 fatty acids linked to a glycerol backbone) without water. So for each day of stored energy we only need to carry 278g or 0.6 lbs. While fat is a slower fuel, in that it takes more time to liberate its energy, many cells with a steady basal energy requirement prefer fat as fuel - heart, intestines, muscles (at low levels of activity). When we eat food, the digestive process breaks it down into its basic components. Fat is broken down into fatty acids which are absorbed, reassembled as fats and distributed to cells that use fat for energy and stored in adipose (fat) tissue. Proteins are broken down into amino acids, distributed to cells that need them and then converted into fat or glucose by the liver depending on our energy needs. Carbohydrates are broken down into glucose, absorbed into the bloodstream triggering the release of insulin from the pancreas. 80-90% of glucose will be stored in the muscles as glycogen, 10% stored in the liver as glycogen with anything extra converted by the liver into fat. So when we eat, we use carbohydrates to top up our glycogen stores and store everything extra as fat. When we are not eating we break down fat into fatty acids providing fuel to the cells that prefer fat, and glycogen into glucose to maintain blood glucose at a steady state. This works well when we are in energy balance. Some days we store a bit more, some days we draw down a bit more. Both energy systems have buffers against overload. The glucose system has a small but immediate buffer through the storage of glucose as glycogen in muscle. The fat system has an immense capacity to buffer excess energy through the storage of fat in subcutaneous adipose tissue. And of course the fat system can buffer the glucose system. With prolonged periods of energy overload these buffers begin to break down. Muscle inactivity results in lower capacity to store glycogen in muscle resulting in more energy being converted into fat. Our ability to store fat in subcutaneous tissue eventually hits a limit. This limit differs greatly amongst different people and is known as the personal fat threshold. We have two ways to store extra fat - store more fat in existing fat cells or create more fat cells. By the time we are 2 years old the number of our subcutaneous fat cells is set. So once these cells are full we have to store fat elsewhere. We retain an ability to create new fat cells in our abdominal space around our intestines and other organs (viscera). This visceral fat is a further attempt to buffer energy overload but it is not without cost, as these fat cells send out inflammatory signals activating our immune system. Fat also begins to build up in other non-fat cells (ectopic fat). As fat builds up in these cells, their ability to respond to insulin decreases; they become insulin resistant. Ectopic fat in muscle results in insulin resistance and muscle takes up less of the glucose from dietary carbohydrates; causing more of this glucose to be converted to fat in the liver. Ectopic fat in the liver also results in insulin resistance. The pancreas initially responds to this insulin resistance by pumping out more insulin both in response to meals but also at baseline to control the liver’s production of glucose in order to maintain normal fasting blood sugars. This increased basal insulin level suppresses the body’s ability to utilize fat for energy as one of insulin’s effects is to inhibit fat oxidation. At this point, weight gain becomes inevitable further compounding the issue. Food is eaten, food is stored, but high levels of insulin prevent the utilization of that stored energy and hunger mechanisms are triggered resulting in more food intake. This extra food energy is in turn stored and the overloaded fat storage system continues to find new, but unhealthy places to store fat: visceral and ectopic fat. This vicious cycle repeats and the problem progresses. Eventually, ectopic fat finds its way into the pancreas and affects insulin production. At this point, insulin production plateaus and can no longer control blood glucose levels. By the time that blood sugars begin to rise - insulin levels are 2-3 times normal levels and 50% of pancreatic beta cells (cells that produce insulin) are dysfunctional. Once fasting blood sugars reach 7.0 mmol/L we call this Type II Diabetes and an estimated 80% of pancreatic beta cells are no longer secreting insulin. The path to Type II Diabetes is the result of sustained energy overload systematically overwhelming our body’s buffers - muscle for glucose and subcutaneous adipose tissue for fat. Over time, excess energy becomes stored as fat in places that it should not be - visceral fat in the abdomen and ectopic fat in cells throughout the body. This fat worsens insulin resistance, resulting in higher insulin levels, and decreasing our ability to use the stored energy driving hunger that adds more energy to an overloaded body. Our individual propensity toward insulin resistance and its manifestation as Type II Diabetes is variable and dependent on such factors as age, genetics, obesity, especially visceral obesity, sedentary behavior, stress, poor sleep and of course poor nutrition.
Learn more about our Diabetes Reversal Programs Previous blog posts: Diabetes Reversal Part I Diabetes Reversal Part II Diabetes Reversal Part III Bessel van der Kolk, MD bestselling author of the Body Keeps The Score is a scientific researcher with a long history of measuring the effects of trauma on brain function, memory, and treatment outcomes, and an active therapist who keeps learning from his patients what benefits them most. In his webcast, Dr. van der Kolk presents the conditions of trauma and describes how we are in a pre-traumatic state where life has become unpredictable and our sense of safety and control feel threatened. Drawing from his experience on working with people who have suffered from trauma- he outlines behaviours that we can do right now in order to protect ourselves from lasting traumatic effects. Trauma lacks predictability: Therefore it is important to create a sense of predictability in our day to day lives by creating structure and planning for experiences to look forward to- i.e. cooking and exercising at predictable times, planning to connect with friends online, etc. Trauma creates a sense of immobility: As humans we have a need to be mobile. Ensure that you are getting enough exercise, create a routine, try activities that involve mind-body connection such as yoga or thai chi. When people experience trauma they lose connection: Make sure you are staying connected with people. Have family dinners, or connect with friends and family online. When out, smile and say hello to strangers as we are all going through this together. You are not alone. Extreme trauma creates a numbing effect or dissociation: Be mindful of the present. Do not numb out the experience through overuse of alcohol or drugs. Go through your day with intention- i.e. plan to cook a new recipe or learn something new. During traumatic experiences we lose our sense of time and sequence: Increase your self awareness by noticing the small changes within yourself and your environment. Notice the present- how you are breathing, how your body feels. Looking outward may feed a sense of hopelessness as the situation is not changing fast enough, but when we look inwards we become aware of ourselves and realize that we are living organisms that are constantly changing. Trauma makes us feel unsafe: Create a sense of safety in your environment by listening to music, eating healthy food, engaging in activities you enjoy, connecting with loved ones if you are sharing your environment with them. Tell yourself that you are safe and that this will pass. Click here for his FREE 25 minute webcast- sign up Condensed version: That which does not kill us, makes us stronger - (Friedrich Nietzsche) ...provided we get enough recovery - (Wellness Garage) Chronic stress can play a central role in the development and progression chronic disease and ill health. But stress is not all bad Let’s consider the paradox of stress Protection and damage are the two contrasting sides of physiological processes that defend our bodies against the challenges of daily life, whether or not we call them “stressors.” We respond to stress in two ways:
Our bodies are designed to respond to a challenge (or stress) by
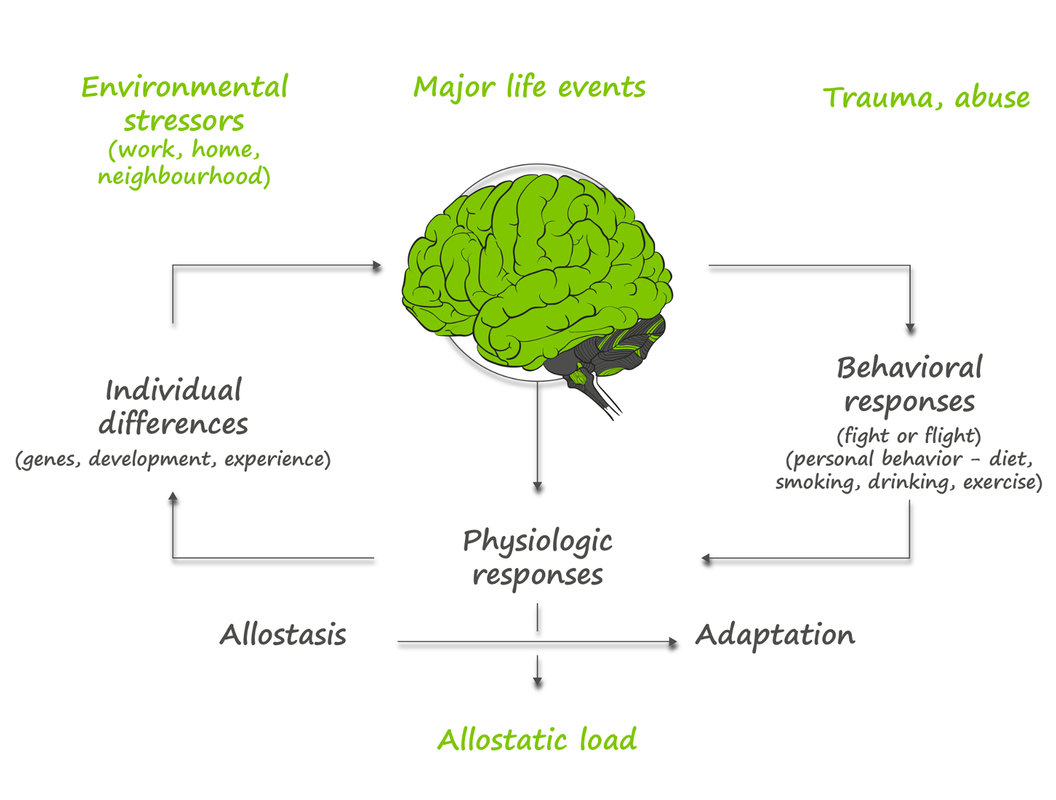
This process is called allostasis – the ability to achieve stability through change. Your response to a stressor is determined by many factors:
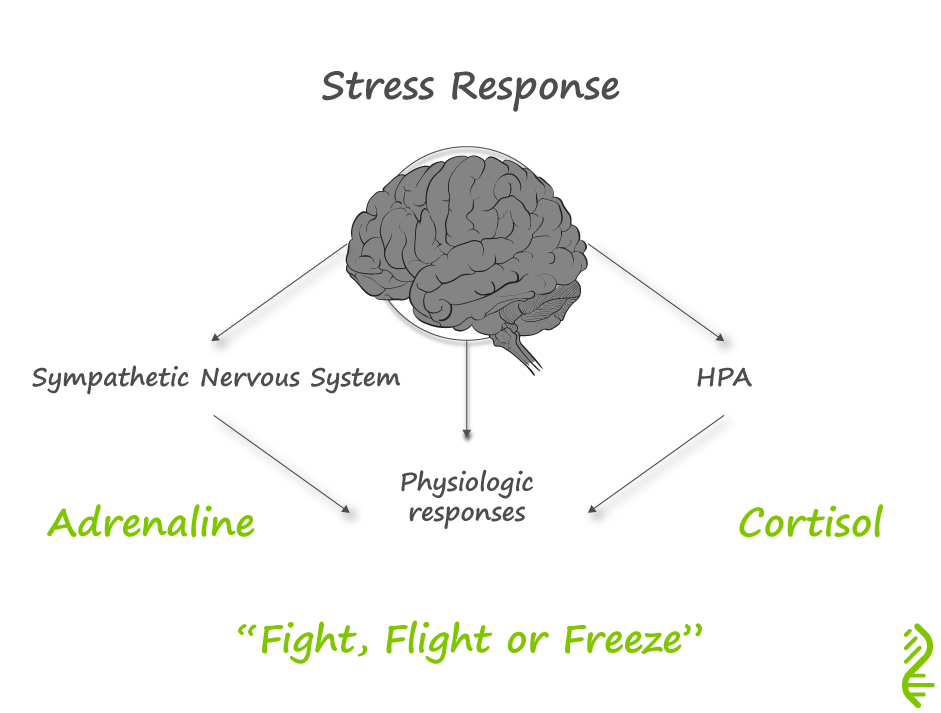
ALL of which determine the extent of your physiological response. Over time allostatic load can accumulate OR the individual can adapt. The immediate stress response is mediated by two systems:
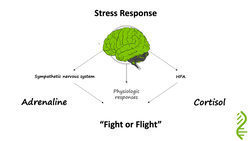 When a situation is perceived as stressful – the hypothalamus sends signals to activate both stress responses. The hypothalamus signals the inner part of the adrenal gland to release adrenaline and which activates the sympathetic nervous system, resulting in:
The effect is immediate and is experienced as the adrenaline rush. The hypothalamus also releases a hormone CRH which activates the pituitary gland to secrete adrenocorticotropic hormone (ACTH) the hormone that stimulates the outer part of the adrenal gland to produce cortisol. Cortisol enables the body to maintain steady supplies of blood sugar for a more prolonged stress. Adequate and steady blood sugar levels help person to cope with prolonged stressor, and helps the body to return to normal. Cortisol does this by:
Once the stress is over the body recovers by:
Every system of the body responds to acute challenge with allostasis leading to adaptation. When these acute responses are overused or inefficiently managed, allostatic overload results. There are 4 patterns to the accumulation of allostatic load:
Remember, three factors largely determine individual responses to potentially stressful situations:
So the key to avoiding the damaging effects of stress is to:
This is why developing stress tolerance is one of our 6 pillars of health Strategies like meditation, yoga, mindfulness, hobbies and anything that brings you into flow can help both the recovery and the perception of stress. Other strategies like ‘stress audits’ can help you identify the areas of life within your control that are causing you stress. Decisions can then be made to alter or avoid these particular situations. Changing your perception of a stressful situation is one of the most powerful ways to develop stress tolerance. Katie Byron has a process called “The Work” in which she walks you through a process that has you answering 4 questions about the situation: Developing a strategy to tolerate stress is a key part of maintaining health - what is your strategy?
|
AuthorDr. Brendan Byrne Categories
All
|







 RSS Feed
RSS Feed
